10.5.6
Pregunta de antecedente 6
En neonatos y niños, ¿qué recomendaciones se deben hacer para tratar la hemorragia crítica?
Evidencia
La definición de hemorragia crítica no está bien establecida en pacientes neonatales y pediátricos. Además, la evidencia sobre qué intervenciones y estrategias tienen los mejores resultados se limita a informes de casos, series de casos, experiencia de un solo centro y pequeños informes retrospectivos (349-352).
Al igual que ocurre con los pacientes adultos, la hemorragia crítica ocurre con mayor frecuencia en escenarios de traumatismos accidentales y no accidentales, cirugías mayores (particularmente cirugías cardíacas y espinales, procedimientos neuroquirúrgicos seleccionados y trasplante hepático) y hemorragia gastrointestinal. En los pacientes neonatos, la exanguinación debida a la hemorragia fetal intraparto o anteparto y la hemorragia subgaleal masiva son afecciones poco comunes, pero están entre las indicaciones para una transfusión de gran volumen.
El Módulo 1 – Sangrado crítico / Transfusión masiva proporciona información general y recomendaciones.
Sin embargo, en general, la evidencia es de nivel bajo y se deriva de estudios sobre poblaciones adultas; por lo tanto, puede no ser directamente aplicable a niños y neonatos
En la población pediátrica, hay variaciones fisiológicas relacionadas con la edad (particularmente en el sistema hemostático) que pueden exacerbar los efectos de sangrado crítico y transfusión de gran volumen. Es probable que estas variaciones fisiológicas tengan el mayor impacto en neonatos, lactantes y niños pequeños.
También hay una marcada variación de la volemia con la edad. Se ha sugerido que la transfusión masiva pediátrica se define como la transfusión de más del 50% del volumen sanguíneo total (VST) en 3 horas, la transfusión de más del 100% VST en 24 horas o el soporte transfusional para reemplazar la pérdida sanguínea de más del 10% VST por minuto (353). Debido a las variaciones en la masa corporal y en el volumen sanguíneo relacionadas con la edad y el peso, los volúmenes de transfusión y el contenido de los paquetes de protocolos de sangrado críticos deben ajustarse por edad o peso (o ambos).
El tratamiento clínico debe tener en cuenta que las soluciones anticoagulantes-conservantes afectan el estado ácido-base y pueden causar hipocalcemia, y que la hipotermia daña la coagulación global (incluyendo la función plaquetaria).
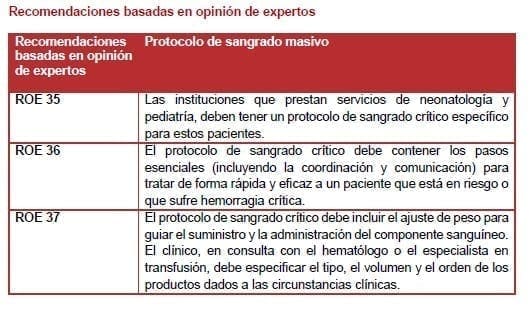
Las instituciones deben desarrollar un protocolo de sangrado crítico específico para pacientes neonatales y pediátricos que tenga en cuenta lo siguiente:
– Orientación sobre cuándo activar
– Quién contactar y cómo contactar con ellos (números de teléfono relevantes)
– Roles y responsabilidades
– Medidas de seguridad rápidas, como usar cánulas de gran calibre cuando sea posible
– Ajustar a la edad o al peso:
- Contenido de los paquetes de protocolos de sangrado críticos
- Volúmenes o dosis de productos sanguíneos utilizados
– Definición de los productos que se incluirán en los paquetes iniciales, secundarios y posteriores (ejemplo: concentrado de glóbulos rojos, PFC, plaquetas y crioprecipitado)
– Indicaciones para el uso del crioprecipitado
– Utilización de las POCT de viscoelasticidad (TEG/ROTEM), definición de su función
– Definición de responsabilidades para la desactivación del protocolo de sangrado crítico, con información de contacto relevante.
Puede ser útil desarrollar protocolos paralelos para el manejo clínico y de laboratorio. Este último debe incluir la dosificación del producto y la administración a la cabecera. La vía clínica debe incluir orientación sobre cuándo realizar las pruebas de laboratorio, qué pruebas a solicitar, interpretación de los resultados y efecto en la selección y dosis del producto.
Referencias
-
1. National Blood Authority (NBA). Patient Blood Management Guidelines: Module 6 – Neonatal and Paediatrics: Technical Report Volume 1-Appendixes, NBA, Canberra, Australia. http://www.blood.gov.au/pbm-module-6
-
2. National Blood Authority (NBA). Patient Blood Management Guidelines: Module 6 – Neonatal and Paediatrics: Technical Report Volume 2 – Annexes, NBA, Canberra, Australia. http://www.blood.gov.au/pbm-module-6
-
3. Kirpalani H and Zupancic JAF. Do transfusions cause necrotizing enterocolitis? The complementary role of randomized trials and observational studies, Seminars in Perinatology 2012; 36(4):269-276. http://www.seminperinat.com/article/S0146-0005(12)00029-8/abstract.
-
4. Mohamed A and Shah PS. Transfusion associated necrotizing enterocolitis: A meta-analysis of observational data, Pediatrics 2012; 129(3):529-540. http://pediatrics.aappublications.org/content/129/3/529.full.pdf
-
5. AlFaleh K, Al-Jebreen A, Baqays A, Al-Hallali A, Bedaiwi K, Al-Balahi N, et al. Association of packed red blood cell transfusion and necrotizing enterocolitis in very low birth weight infants, J Neonatal Perinatal Med 7 2014; (3):193-198. http://www.ncbi.nlm.nih.gov/pubmed/25318632
-
6. Baer VL, Lambert DK, Henry E, Snow GL, Butler A and Christensen RD. Among very-low-birth-weight neonates is red blood cell transfusion an independent risk factor for subsequently developing a severe intraventricular hemorrhage?, Transfusion 2011; 51(6):1170-1178. http://onlinelibrary.wiley.com/doi/10.1111/j.1537-2995.2010.02980.x/abstract
-
7. Demirel G, Celik IH, Aksoy HT, Erdeve O, Oguz SS, Uras N, et al. Transfusion-associated necrotising enterocolitis in very low birth weight premature infants, Transfusion Medicine 2012, 22(5):332-337. http://onlinelibrary.wiley.com/doi/10.1111/j.1365-3148.2012.01170.x/abstract
-
8. Dos Santos AMN, Guinsburg R, De Almeida MFB, Procianoy RS, Leone CR, Marba STM, et al. Red blood cell transfusions are independently associated with intra-hospital mortality in very low birth weight preterm infants, Journal of Pediatrics 2011; 159(3):371-376. http://www.sciencedirect.com/science/article/pii/S0022347611002459
-
9. Elabiad MT, Harsono M, Talati AJ and Dhanireddy R. Effect of birth weight on the association between necrotising enterocolitis and red blood cell transfusions in (less-than or equal to) 1500 g infants, BMJ Open 2013, 3(11). http://dx.doi.org/10.1136/bmjopen-2013-003823
-
10. Feghhi M, Altayeb SMH, Haghi F, Kasiri A, Farahi F, Dehdashtyan M, et al. Incidence of retinopathy of prematurity and risk factors in the South-Western Region of Iran, Middle East African Journal of Ophthalmology 2012; 19(1):101-106. http://www.meajo.org/article.asp?issn=0974-9233;year=2012;volume=19;issue=1;spage=101;ep age=106;aulast=Feghhi
-
11. Fortes Filho JB, Borges Fortes BG, Tartarella MB and Procianoy RS. Incidence and main risk factors for severe retinopathy of prematurity in infants weighing less than 1000 grams in Brazil, Journal of Tropical Pediatrics 2013; 59(6):502-506. http://dx.doi.org/10.1093/tropej/fmt036
-
12. Hakeem A, Mohamed GB and Othman MF. Retinopathy of prematurity: A study of incidence and risk factors in NICU of Al-Minya University Hospital in Egypt, Journal of Clinical Neonatology 2012; 1(2):76-81. http://dx.doi.org/10.4103/2249-4847.96755
-
13. Kabatas EU, Beken S, Aydin B, Dilli D, Zenciroglu A and Okumus N. The risk factors for retinopathy of prematurity and need of laser photocoagulation: A single center experience, Gazi Medical Journal 24(4). http://dx.doi.org/10.12996/gmj.2013.31
-
14. Li ML, Hsu SM, Chang YS, Shih MH, Lin YC, Lin CH, et al. bRetinopathy of prematurity in southern Taiwan: A 10-year tertiary medical center study, Journal of the Formosan Medical Association 2013; 112(8):445-453. http://www.jfma-online.com/article/S0929-6646(12)00236-7/pdf
-
15. Navaei F, Aliabady B, Moghtaderi J, Moghtaderi M and Kelishadi R. Early outcome of preterm infants with birth weight of 1500 g or less and gestational age of 30 weeks or less in Isfahan city, Iran, World J Pediatr 2010; 6(3):228-232.} http://www.ncbi.nlm.nih.gov/pubmed/20549417
-
16. Stritzke AI, Smyth J, Synnes A, Lee SK and Shah PS. Transfusion-associated necrotising enterocolitis in neonates, Archives of Disease in Childhood: Fetal and Neonatal Edition 2013; 98(1):F10-F14. http://fn.bmj.com/content/98/1/F10.long
-
17. Wan-Huen P, Bateman D, Shapiro DM and Parravicini E. Packed red blood cell transfusion is an independent risk factor for necrotizing enterocolitis in premature infants, Journal of Perinatology 2013; 33(10):786-790. http://dx.doi.org/10.1038/jp.2013.60
-
18. Weintraub Z, Carmi N, Elouti H and Rumelt S. The association between stage 3 or higher retinopathy of prematurity and other disorders of prematurity, Canadian Journal of Ophthalmology 2011; 46(5):419-424. http://www.canadianjournalofophthalmology.ca/article/S0008-4182(11)00166-9/abstract
-
19. Bassler D, Weitz M, Bialkowski A and Poets CF. Restrictive versus liberal red blood cell transfusion strategies for preterm infants: A systematic review of randomized controlled trials, Current Pediatric Reviews 2008; 4(3):143-150. http://dx.doi.org/10.2174/157339608785855983
-
20. Ibrahim M, Ho SKY and Yeo CL. Restrictive versus liberal red blood cell transfusion thresholds in very low birth weight infants: A systematic review and meta-analysis, Journal of Paediatrics and Child Health 2014; 50(2):122-130. http://dx.doi.org/10.1111/jpc.12409
-
21. Venkatesh V, Khan R, Curley A, Hopewell S, Doree C and Stanworth S. The safety and efficacy of red cell transfusions in neonates: A systematic review of randomized controlled trials, Br J Haematol 2012, 158(3):370-385.
-
22. Whyte R and Kirpalani H. Low versus high haemoglobin concentration threshold for blood transfusion for preventing morbidity and mortality in very low birth weight infants, Cochrane database of systematic reviews (Online) 2011; (11):CD000512. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L560067527
-
23. Bell EF, Strauss RG, Widness JA, Mahoney LT, Mock DM, Seward VJ, et al. Randomized trial of liberal versus restrictive guidelines for red blood cell transfusion in preterm infants, Pediatrics 2005; 115(6):1685-1691. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2866196/pdf/nihms-199759.pdf
-
24. Chen HL, Tseng HI, Lu CC, Yang SN, Fan HC and Yang RC. Effect of Blood Transfusions on the Outcome of Very Low Body Weight Preterm Infants under Two Different Transfusion Criteria, Pediatrics and Neonatology 2009; 50(3):110-116. http://www.pediatr-neonatol.com/article/S1875-9572(09)60045-0/pdf
-
25. Kirpalani H, Whyte RK, Andersen C, Asztalos EV, Heddle N, Blajchman MA, et al. The premature infants in need of transfusion (pint) study: A randomized, controlled trial of a restrictive (LOW) versus liberal (HIGH) transfusion threshold for http://www.jpeds.com/article/S0022-3476(06)00444-6/abstract
-
26. Brooks SE, Marcus DM, Gillis D, Pirie E, Johnson MH and Bhatia J (1999). The effect of blood transfusion protocol on retinopathy of prematurity: A prospective, randomized study, Pediatrics 1999; 104(3 I):514-518.
-
27. Connelly RJ, Stone SH and Whyte RK. Early vs. late red cell transfusion in low birth weight infants, Pediatr Res 1998; 43(4):170A.
-
28. Whyte RK, Kirpalani H, Asztalos EV, Andersen C, Blajchman M, Heddle N, et al. Neurodevelopmental outcome of extremely low birth weight infants randomly assigned to restrictive or liberal hemoglobin thresholds for blood transfusion, Pediatrics 2009; 123(1):207-213. http://pediatrics.aappublications.org/content/123/1/207.long
-
29. Boost II United Kingdom Collaborative Group, Boost II Australia Collaborative Group, Boost II New Zealand Collaborative Group, Stenson BJ, Tarnow-Mordi WO, Darlow BA, et al. Oxygen saturation and outcomes in preterm infants, N Engl J Med 2013; 368(22):2094–2104. http://www.ncbi.nlm.nih.gov/pubmed/23642047
-
30. (2015). Transfusion of Prematures (TOP) Trial. https://clinicaltrials.gov/ct2/show/NCT01702805
-
31. Effects of transfusion thresholds on neurocognitive outcome of extremely low birth weight infants (ETTNO). http://www.medizin.uni-tuebingen.de/kinder/en/departments/cpcs/projekte/ETTNO_ Information_HomepageCPCS_AF.pdf
-
32. Carson JL, Grossman BJ, Kleinman S, Tinmouth AT, Marques MB, Fung MK, et al. Red blood cell transfusion: a clinical practice guideline from the AABB, Annals of Internal Medicine 2012; 157(1):49- 58. http://annals.org/data/Journals/AIM/24329/0000605-201207030-00008.pdf
-
33. Lacroix J, Hebert PC, Hutchison JS, Hume HA, Tucci M, Ducruet T, et al. Transfusion strategies for patients in pediatric intensive care units, New England Journal of Medicine 2007; 356(16):1609-1619. http://www.nejm.org/doi/pdf/10.1056/NEJMoa066240
-
34. Adams RJ, McKie VC, Hsu L, Beatrice F, Vichinsky E, Pegelow C, et al. Prevention of a first stroke by transfusions in children with sickle cell anemia and abnormal results on transcranial Doppler ultrasonography, New England Journal of Medicine 1998; 339(1):5-11. http://www.nejm.org/doi/pdf/10.1056/NEJM199807023390102
-
35. Debaun MR, Gordon M, McKinstry RC, Noetzel MJ, White DA, Sarnaik SA, et al. Controlled trial of transfusions for silent cerebral infaECAs in sickle cell anemia, New England Journal of Medicine 2014; 371(8):699-710. http://www.nejm.org/doi/pdf/10.1056/NEJMoa1401731
-
36. Pegelow CH, Macklin EA, Moser FG, Wang WC, Bello JA, Miller ST, et al. Longitudinal changes in brain magnetic resonance imaging findings in children with sickle cell disease, Blood 2002; 99(8):3014–3018. http://www.ncbi.nlm.nih.gov/pubmed/11929794
-
37. Bernaudin M, Bellail A, Marti HH, Yvon A, Vivien D, Duchatelle I, et al. Neurons and astrocytes express EPO mRNA: oxygen-sensing mechanisms that involve the redox-state of the brain, Glia 2000; 30(3):271–278. http://www.ncbi.nlm.nih.gov/pubmed/10756076
-
38. Cherry MG, Greenhalgh J, Osipenko L, Venkatachalam M, Boland A, Dundar Y, et al. The clinical effectiveness and cost-effectiveness of primary stroke prevention in children with sickle cell disease: A Systematic Review and Economic Evaluation, Health Technology Assessment 2012; 16(43):1-129. http://dx.doi.org/10.3310/hta16430
-
39. Wang WC and Dwan K. Blood transfusion for preventing primary and secondary stroke in people with sickle cell disease, Cochrane Database of Systematic Reviews. 2013
-
40. Adams RJ and Brambilla D. Discontinuing prophylactic transfusions used to prevent stroke in sickle cell disease, New England Journal of Medicine 2005; 353(26):2769-2778. http://www.nejm.org/doi/pdf/10.1056/NEJMoa050460
-
41. Pegelow CH, Wang W, Granger S, Hsu LL, Vichinsky E, Moser FG, et al. Silent infaECAs in children with sickle cell anemia and abnormal cerebral artery velocity, Archives of Neurology 2001; 58(12):2017-2021. http://archneur.jamanetwork.com/data/Journals/NEUR/6833/NOC10072.pdf
-
42. US Department of Health and Human Services and National Institutes of Health (NIH) (2014). Evidence-based management of sickle cell disease: Expert panel report, Bethesda, USA. https://www.nhlbi.nih.gov/health-pro/guidelines/sickle-cell-disease-guidelines
-
43. DTC With Transfusions Changing to Hydroxyurea (TWiTCH): A Phase III Randomized Clinical Trial to Compare Standard Therapy (Erythrocyte Transfusions) With Alternative Therapy (Hydroxyurea) for the Maintenance of Lowered DTC Velocities in Pediatric Subjects With Sickle Cell Anemia and Abnormal Pre-treatment DTC Velocities. ttps://clinicaltrials.gov/ct2/show/study/NCT01425307?term=Twitch+sickle+cell&rank=1
-
44. Masera G, Terzoli S, Avanzini A, Fontanelli G, Mauri RA, Piacentini G, et al. Evaluation of the supertransfusion regimen in homozygous beta-thalassaemia children, Br J Haematol 1982; 52(1):111– 113. http://www.ncbi.nlm.nih.gov/pubmed/7115620
-
45. Cazzola M, Borgna-Pignatti C, Locatelli F, Ponchio L, Beguin Y and De Stefano P. A moderate transfusion regimen may reduce iron loading in beta-thalassemia major without producing excessive expansion of erythropoiesis, Transfusion 1997; 37(2):135–140. http://www.ncbi.nlm.nih.gov/pubmed/9051086
-
46. Torcharus K, Withayathawornwong W, Sriphaisal T, Krutvacho T, Arnutti P and Suwanasophorn C. High transfusion in children with beta-thalassemia/Hb E: clinical and laboratory assessment of 18 cases, Southeast Asian J Trop Med Public Health 1993; 24 (1):96–99. http://www.ncbi.nlm.nih.gov/pubmed/7886617
-
47. Jaime-Perez JC, Colunga-Pedraza PR and Gomez-Almaguer D. Is the number of blood products transfused associated with lower survival in children with acute lymphoblastic leukemia?, Peditric Blood and Cancer 2011; 57(2):217-223. http://dx.doi.org/10.1002/pbc.22957
-
48. Kneyber MCJ, Grotenhuis F, Berger RFM, Ebels TW, Burgerhof JGM and Albers MJIJ. Transfusion of leukocyte-depleted RBCs is independently associated with increased morbidity after pediatric cardiac surgery, Pediatric Critical Care Medicine 2013; 14(3):298-305. http://dx.doi.org/10.1097/PCC.0b013e3182745472
-
49. Nacoti M, Cazzaniga S, Lorusso F, Naldi L, Brambillasca P, Benigni A, et al. The impact of perioperative transfusion of blood products on survival after pediatric liver transplantation, Pediatric Transplantation 2012; 16(4):357-366. http://www.ncbi.nlm.nih.gov/pubmed/22429563
-
50. Redlin M, Kukucka M, Boettcher W, Schoenfeld H, Huebler M, Kuppe H, et al. Blood transfusion determines postoperative morbidity in pediatric cardiac surgery applying a comprehensive blood-sparing approach, Journal of Thoracic and Cardiovascular Surgery 2013; 146(3):537-542. http://www.jtcvsonline.org/article/S0022-5223(12)01432-8/abstract
-
51. Wilkinson KL, Brunskill SJ, Doree C, Trivella M, Gill R and Murphy MF (2014). Red cell transfusion management for patients undergoing cardiac surgery for congenital heart disease, Cochrane Database of Systematic Reviews.
-
52. Cholette JM, Rubenstein JS, Alfieris GM, Powers KS, Eaton M and Lerner NB. Children with single-ventricle physiology do not benefit from higher hemoglobin levels post cavopulmonary connection: Results of a prospective, randomized, controlled trial of a restrictive versus liberal red- cell transfusion strategy, Pediatric Critical Care Medicine 2011; 12(1):39-45. http://dx.doi.org/10.1097/PCC.0b013e3181e329db
-
53. Willems A, Harrington K, Lacroix J, Biarent D, Joffe AR, Wensley D, et al. Comparison of two red-cell transfusion strategies after pediatric cardiac surgery: A subgroup analysis, Critical Care Medicine 2010; 38(2):649-656. http://dx.doi.org/10.1097/CCM.0b013e3181bc816c
-
54. Rouette J, Trottier H, Ducruet T, Beaunoyer M, Lacroix J and Tucci M. Red blood cell transfusion threshold in postsurgical pediatric intensive care patients: A randomized clinical trial, Annals of Surgery 2010; 251(3):421-427. http://dx.doi.org/10.1097/SLA.0b013e3181c5dc2e
-
55. Robitaille N, Lacroix J, Alexandrov L, Clayton L, Cortier M, Schultz KR, et al. Excess of Veno- Occlusive Disease in a Randomized Clinical Trial on a Higher Trigger for Red Blood Cell Transfusion after Bone Marrow Transplantation: A Canadian Blood and Marrow Transplant Group Trial, Biology of Blood and Marrow Transplantation 2013; 19(3):468-473. http://www.bbmt.org/article/S1083-8791(12)01138-X/pdf
-
56. Acker SN, Partrick DA, Ross JT, Nadlonek NA, Bronsert M and Bensard DD. Blood component transfusion increases the risk of death in children with traumatic brain injury, Journal of Trauma and Acute Care Surgery 2014; 76(4):1082-1088. http://dx.doi.org/10.1097/TA.0000000000000095
-
57. Fremgen HE, Bratton SL, Metzger RR and Barnhart DC. Pediatric liver lacerations and intensive care: Evaluation of ICU triage strategies, Pediatric Critical Care Medicine 2014; 15(4):e183-e191. http://dx.doi.org/10.1097/PCC.0000000000000102
-
58. Hassan NE, DeCou JM, Reischman D, Nickoles TA, Gleason E, Ropele DL, et al. GR transfusions in children requiring intensive care admission after traumatic injury, Pediatric Critical Care Medicine 2014; 15(7):e306-313. http://dx.doi.org/10.1097/PCC.0000000000000192
-
59. Carson JL, Carless PA and Hebert PC (2012). Transfusion thresholds and other strategies for guiding allogeneic red blood cell transfusion, Cochrane Database of Systematic Reviews (4).
-
60. Desjardins P, Turgeon AF, Tremblay MH, Lauzier F, Zarychanski R, Boutin A, et al. Hemoglobin levels and transfusions in neurocritically ill patients: A systematic review of comparative studies, Crit Care 2012; 16(2). http://dx.doi.org/10.1186/cc11293
-
61. Aher SM and Ohlsson A (2012). Late erythropoietin for preventing red blood cell transfusion in preterm and/or low birth weight infants, Cochrane database of systematic reviews 9:CD004868.
-
62. Garcia MG, Hutson AD and Christensen RD. Effect of recombinant erythropoietin on”late” transfusions in the neonatal intensive care unit: A meta-analysis, Journal of Perinatology 2002; 22(2):108-111. http://www.nature.com/jp/journal/v22/n2/pdf/7210677a.pdf
-
63. Kotto-Kome AC, Garcia MG, Calhoun DA and Christensen RD. Effect of beginning recombinant erythropoietin treatment within the first week of life, among very-low-birth-weight neonates, on ”early” and ”late” erythrocyte transfusions: A meta-analysis, Journal of Perinatology 2004; 24(1):24-29. http://www.nature.com/jp/journal/v24/n1/pdf/7211018a.pdf
-
64. Ohlsson A and Aher SM. Early erythropoietin for preventing red blood cell transfusion in preterm and/or low birth weight infants, Cochrane database of systematic reviews (Online) 2012; 9:CD004863.
-
65. Vamvakas EC and Strauss. Meta-analysis of controlled clinical trials studying the efficacy of rHuEPO in reducing blood transfusions in the anemia of prematurity, Transfusion 2001; 41(3):406-415. http://onlinelibrary.wiley.com/doi/10.1046/j.1537-2995.2001.41030406.x/abstract
-
66. Xu XJ, Huang HY and Chen HL. Erythropoietin and retinopathy of prematurity: a meta- analysis, European Journal of Pediatrics 2014; 173(10):1355-1364. http://dx.doi.org/10.1007/s00431-014-2332-4
-
67. El-Ganzoury MM, Awad HA, El-Farrash RA, El-Gammasy TM, Ismail EA, Mohamed HE, et al. Enteral Granulocyte-Colony Stimulating Factor and Erythropoietin Early in Life Improves Feeding Tolerance in Preterm Infants: A Randomized Controlled Trial, Journal of Pediatrics 2014; 165(6):1140- 1145. http://dx.doi.org/10.1016/j.jpeds.2014.07.034
-
68. Jim WT, Chen LT, Huang FY and Shu CH. The early use of recombinant human erythropoietin in anemia of prematurity, Clinical Neonatology 2000; 7(2):12-16. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L47248848
-
69. Kremenopoulos G, Soubasi V, Tsantali C, Diamanti E and Tsakiris D.The best timing of recombinant human erythropoietin administration in anemia of prematurity: A randomized controlled study, International Journal of Pediatric Hematology/Oncology 1987; 4(4):373-383. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L27501001
-
70. Ovali F, Samanci N and Dagoglu T. Management of late anemia in rhesus hemolytic disease: Use of recombinant human erythropoietin (a pilot study), Pediatr Res 1996; 39(5):831-834.
-
71. Aher SM and Ohlsson A. Late erythropoietin for preventing red blood cell transfusion in preterm and/or low birth weight infants, Cochrane database of systematic reviews 2014, 4:CD004868. http://www.ncbi.nlm.nih.gov/pubmed/24760628
-
72. Ohlsson A and Aher SM (2014). Early erythropoietin for preventing red blood cell transfusion in preterm and/or low birth weight infants, Cochrane database of systematic reviews 4:CD004863. http://www.ncbi.nlm.nih.gov/pubmed/24771408
-
73. Collard KJ.Iron homeostasis in the neonate, Pediatrics 2009, 123(4):1208-1216. http://www.ncbi.nlm.nih.gov/pubmed/19336381
-
74. Friel JK, Andrews WL, Aziz K, Kwa PG, Lepage G and L’Abbe MR. A randomized trial of two levels of iron supplementation and developmental outcome in low birth weight infants, J Pediatr 2001; 139(2):254-260. http://www.ncbi.nlm.nih.gov/pubmed/11487753
-
75. Friel JK, Andrews WL, Aziz K, Kwa PG, Lepage G and L’Abbe MR. A randomized trial of two levels of iron supplementation and developmental outcome in low birth weight infants, J Pediatr 2001; 139(2):254-260. http://www.ncbi.nlm.nih.gov/pubmed/11487753
-
76. Long H, Yi JM, Hu PL, Li ZB, Qiu WY, Wang F, et al. Benefits of iron supplementation for low birth weight infants: a systematic review, BMC Pediatr 2012, 12:99. http://www.ncbi.nlm.nih.gov/pubmed/22794149
-
77. Taylor TA and Kennedy KA. Randomized trial of iron supplementation versus routine iron intake in VLBW infants, Pediatrics 2013; 131(2):e433-e438. http://pediatrics.aappublications.org/content/131/2/e433.full.pdf
-
78. Sankar MJ, Saxena R, Mani K, Agarwal R, Deorari AK and Paul VK. Early iron supplementation in very low birth weight infants – A randomized controlled trial, Acta Paediatrica, International Journal of Paediatrics 2009; 98(6):953-958. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L354556418
-
79. Berseth CL, Van Aerde JE, Gross S, Stolz SI, Harris CL and Hansen JW. Growth, efficacy, and safety of feeding an iron-fortified human milk fortifier, Pediatrics 2004; 114(6):e699-706. http://www.ncbi.nlm.nih.gov/pubmed/15545616
-
80. Franz AR, Mihatsch WA, Sander S, Kron M and Pohlandt F. Prospective randomized trial of early versus late enteral iron supplementation in infants with a birth weight of less than 1301 grams, Pediatrics 2000; 106(4):700-706. http://www.ncbi.nlm.nih.gov/pubmed/11015511
-
81. Agostoni C, Buonocore G, Carnielli VP, De Curtis M, Darmaun D, Decsi T, et al. Enteral nutrient supply for preterm infants: commentary from the European Society of Paediatric Gastroenterology, Hepatology and Nutrition Committee on Nutrition, J Pediatr Gastroenterol Nutr 2010; 50(1):85-91. http://www.ncbi.nlm.nih.gov/pubmed/19881390
-
82. Kleinman R and Greer F (Eds.) (2014). Pediatric Nutrition Handbook, 7th edition, American Academy of Pediatrics Committee on Nutrition, Elk Grove Village, IL.
-
83. asricha SR, Hayes E, Kalumba K and Biggs BA. Effect of daily iron supplementation on health in children aged 4-23 months: A systematic review and meta-analysis of randomised controlled trials, The Lancet Global Health 2013; 1(2):e77-e86. http://www.thelancet.com/pdfs/journals/langlo/PIIS2214-109X(13)70046-9.pdf
-
84. Okebe JU, Yahav D, Shbita R and Paul M (2011). Oral iron supplements for children in malaria-endemic areas, Cochrane database of systematic reviews (10):CD006589. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L362839424
-
85. National Blood Authority (NBA) (2012). Patient Blood Management Guidelines: Module 3 – Medical, NBA, Canberra, Australia. http://www.blood.gov.au/pbm-module-3
-
86. Feusner J and Hastings C. Recombinant human erythropoietin in pediatric oncology: a review (Structured abstract), Medical and Pediatric Oncology 2002; 39:463-468. http://onlinelibrary.wiley.com/doi/10.1002/mpo.10187/abstract
-
87. Grant MD, Piper M, Bohlius J, Tonia T, Robert N, Vats V, et al. (2013). Epoetin and darbepoetin for managing anemia in patients undergoing cancer treatment: comparative effectiveness update, Comparative Effectiveness Review No. 113, Agency for Healthcare Research and Quality, Rockville, MD.
-
88. Mystakidou K, Potamianou A and Tsilika E. Erythropoietic growth factors for children with cancer: A systematic review of the literature, Current Medical Research and Opinion 2007; 23(11): 2841-2847. http://informahealthcare.com/doi/abs/10.1185/030079907X242601%20
-
89. Ross SD, Allen IE, Henry DH, Seaman C, Sercus B and Goodnough LT. Clinical enefits and risks associated with epoetin and darbepoetin in patients with chemotherapy-induced anemia: a systematic review of the literature (Structured abstract), Clinical Therapeutics 2006; 28:801-831.} http://www.clinicaltherapeutics.com/article/S0149-2918(06)00139-1/abstract
-
90. Tonia T, Mettler A, Robert N, Schwarzer G, Seidenfeld J, Weingart O, et al. (2012). Erythropoietin or darbepoetin for patients with cancer, Cochrane database of systematic reviews (12). http://onlinelibrary.wiley.com/doi/10.1002/14651858.CD003407.pub5/pdf
-
91. Bennetts G, Bertolone S, Bray G. Erythropoietin reduces volume of red cell transfusions required in some subsets of children with acute lymphocytic leukemia [abstract], Blood 1995,10:853.
-
92. Csaki C, Ferencz T, Schuler D and Borsi J. Recombinant human erythropoietin in the prevention of chemotherapy-induced anaemia in children with malignant solid tumours, European Journal of Cancer 1998; 34(3):364-367. http://www.sciencedirect.com/science/article/pii/S095980499710065X
-
93. Porter JC, Leahey A, Polise K, Bunin G and Manno CS. Recombinant human erythropoietin reduces the need for erythrocyte and platelet transfusions in pediatric patients with sarcoma: a randomized, double-blind, placebo-controlled trial, J Pediatr 1996; 129(5):656-660. http://www.ncbi.nlm.nih.gov/pubmed/8917229
-
94. Ragni G, Clerico A, Sordi A and et al. Recombinant human erythropoietin (rHuEPO) in children with cancer: A randomized study [abstract], Med Pediatr Oncol 1998, 31:274.
-
95. Razzouk BI, Hord JD, Hockenberry M, Hinds PS, Feusner J, Williams D, et al. Double-blind, placebo-controlled study of quality of life, hematologic end points, and safety of weekly epoetin alfa in children with cancer receiving myelosuppressive chemotherapy, J Clin Oncol 2006, 24(22): 3583-3589. http://www.ncbi.nlm.nih.gov/pubmed/16877725
-
96. Varan A, Büyükpamukçu M, Kutluk T and Akyüz C. Recombinant human erythropoietin treatment for chemotherapy-related anemia in children, Pediatrics 1999; 103(2):e16-e16. http://pediatrics.aappublications.org/content/103/2/e16.short
-
97. Wagner LM, Billups CA, Furman WL, Rao BN and Santana VM. Combined use of erythropoietin and granulocyte colony-stimulating factor does not decrease blood transfusion requirements during induction therapy for high-risk neuroblastoma: a randomized controlled trial, Journal of clinical oncology 2004; 22(10):1886-1893. http://jco.ascopubs.org/content/22/10/1886.short
-
98. Kidney Disease: Improving Global Outcomes (KDIGO) Anemia Work Group. KDIGO Clinical practice guideline for anemia in chronic kidney disease, Kidney Int 2012; 2(4):279–335. http://kdigo.org/home/guidelines/anemia-in-ckd/
-
99. National Institute for Health and Care Excellence (NICE) (2011). Anaemia management in people with chronic kidney disease, NICE, UK. http://www.nice.org.uk/guidance/cg114
-
100. Cody J, Daly C, Campbell M, Donaldson C, Khan I, Rabindranath K, et al. (2005). Recombinant human erythropoietin for chronic renal failure anaemia in pre-dialysis patients, Cochrane database of systematic reviews (3):CD003266. http://www.ncbi.nlm.nih.gov/pubmed/16034896
-
101. Pape L, Ahlenstiel T, Kreuzer M, Drube J, Froede K, Franke D, et al. Early erythropoietin reduced the need for red blood cell transfusion in childhood hemolytic uremic syndrome – A randomized prospective pilot trial, Pediatric Nephrology 2009; 24(5):1061-1064. http://link.springer.com/article/10.1007%2Fs00467-008-1087-4
-
102. National Institute for Health and Care Excellence (NICE) (2015). Anaemia management in people with chronic kidney disease, NICE, UK. http://www.nice.org.uk/guidance/ng8/resources/anaemia-management-in-people- withchronic- kidney-disease-51046844101
-
103. Albaramki J, Hodson EM, Craig JC and Webster AC (2012). Parenteral versus oral iron therapy for adults and children with chronic kidney disease, Cochrane Database Syst Rev 1:CD007857. http://www.ncbi.nlm.nih.gov/pubmed/22258974
-
104. Warady BA, Kausz A, Lerner G, Brewer ED, Chadha V, Brugnara C, et al. Iron therapy in the pediatric hemodialysis population, Pediatric Nephrology 2004; 19(6):655-661. http://link.springer.com/article/10.1007%2Fs00467-004-1457-5
-
105. Voskaridou E, Christoulas D, Bilalis A, Plata E, Varvagiannis K, Stamatopoulos G, et al. The effect of prolonged administration of hydroxyurea on morbidity and mortality in adult patients with sickle cell syndromes: results of a 17-year, single-center trial (LaSHS), Blood 2010; 115(12): 2354-2363. http://www.ncbi.nlm.nih.gov/pubmed/19903897
-
106. Jones AP, Davies S and Olujohungbe A (2001). Hydroxyurea for sickle cell disease, Cochrane database of systematic reviews (2):CD002202. http://onlinelibrary.wiley.com/doi/10.1002/14651858.CD002202/epdf
-
107. Mulaku M, Opiyo N, Karumbi J, Kitonyi G, Thoithi G and English M. Evidence review of hydroxyurea for the prevention of sickle cell complications in low-income countries, Archives of Disease in Childhood 2013; 98(11):908–914. http://adc.bmj.com/content/98/11/908.full.pdf
-
108. Segal JB, Strouse JJ, Beach MC, Haywood C, Witkop C, Park H, et al. Hydroxyurea for the treatment of sickle cell disease, Evid Rep Technol Assess (Full Rep) 2008; (165):1-95. http://www.ncbi.nlm.nih.gov/pubmed/18457478
-
109. Jain DL, Sarathi V, Desai S, Bhatnagar M and Lodha A. Low fixed-dose hydroxyurea in severely affected Indian children with sickle cell disease, Hemoglobin 2012; 36(4):323-332. http://informahealthcare.com/doi/abs/10.3109/03630269.2012.697948
-
110. Wang WC, Ware RE, Miller ST, Iyer RV, Casella JF, Minniti CP, et al. Hydroxycarbamide in very young children with sickle-cell anaemia: A multicentre, randomised, controlled trial (BABY HUG), The Lancet 2011; 377(9778):1663-1672. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3133619/pdf/nihms298546.pdf
-
111. Andropoulos DB, Brady K, Easley RB, Dickerson HA, Voigt RG, Shekerdemian LS, et al. Erythropoietin neuroprotection in neonatal cardiac surgery: A phase I/II safety and efficacy trial, Journal of Thoracic and Cardiovascular Surgery 2013; 146(1):124-131. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3579008/pdf/nihms417782.pdf
-
112. Bierer R, Roohi M, Peceny C and Ohls RK. Erythropoietin increases reticulocyte counts and maintains hematocrit in neonates requiring surgery, Journal of Pediatric Surgery 2009; 44(8):1540-1545. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3086684/pdf/nihms281836.pdf
-
113. Fearon JA and Weinthal J. The use of recombinant erythropoietin in the reduction of blood transfusion rates in craniosynostosis repair in infants and children, Plastic and Reconstructive Surgery 2002; 109(7):2190-2196. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L34556189
-
114. National Blood Authority (NBA) (2012). Patient Blood Management Guidelines: Module 2 – Perioperative, NBA, Canberra, Australia. http://www.blood.gov.au/pbm-module-2
-
115. Jacobs BR, Lyons K and Brilli RJ.Erythropoietin therapy in children with bronchiolitis and anemia, Pediatric critical care medicine: a journal of the Society of Critical Care Medicine and the World Federation of Pediatric Intensive and Critical Care Societies 2003; 4(1):44-48. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L36652247
-
116. Osborn DA and Evans N (2004). Early volume expansion for prevention of morbidity and mortality in very preterm infants, Cochrane database of systematic reviews (Online) (2):CD002055. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L39041654
-
117. The Northern Neonatal Nursing Initiative Trial G. A randomized trial comparing the effect of prophylactic intravenous fresh frozen plasma, gelatin or glucose on early mortality and morbidity in preterm babies, 1996a; 155:580-588.
-
118. The Northern Neonatal Nursing Initiative Trial G. Randomised trial of prophylactic early fresh-frozen plasma or gelatin or glucose in preterm babies: outcome at 2 years, 1996b 348:229-232.
-
119. Baer VL, Lambert DK, Henry E, Snow GL, Sola-Visner MC and Christensen RD. Do platelet transfusions in the NICU adversely affect survival? Analysis of 1600 thrombocytopenic neonates in a multihospital healthcare system, Journal of Perinatology 2007; 27(12):790-796. http://www.ncbi.nlm.nih.gov/pubmed/17855804
-
120. Bonifacio L, Petrova A, Nanjundaswamy S and Mehta R. Thrombocytopenia related neonatal outcome in preterms, Indian Journal of Pediatrics 2007; 74(3):267-274. http://www.ncbi.nlm.nih.gov/pubmed/17401266
-
121. Christensen RD, Henry E, Wiedmeier SE, Stoddard RA, Sola-Visner MC, Lambert DK, et al. Thrombocytopenia among extremely low birth weight neonates: Data from a multihospital healthcare system, Journal of Perinatology 2006; 26(6):348-353. http://www.ncbi.nlm.nih.gov/pubmed/16642027
-
122. Von Lindern JS, Hulzebos CV, Bos AF, Brand A, Walther FJ and Lopriore E. Thrombocytopaenia and intraventricular haemorrhage in very premature infants: A tale of two cities, Arch Dis Child Fetal Neonatal Ed 2012; 97(5):F348-352. http://fn.bmj.com/content/97/5/F348.long
-
123. Curley A, Venkatesh V, Stanworth S, Clarke P, Watts T, New H, et al. Platelets for neonatal transfusion – study 2: a randomised controlled trial to compare two different platelet count thresholds for prophylactic platelet transfusion to preterm neonates, Neonatology 2014; 106(2): 102-106. http://www.ncbi.nlm.nih.gov/pubmed/24851997
-
124. Estcourt L, Stanworth S, Doree C, Hopewell S, Murphy MF, Tinmouth A, et al. Prophylactic platelet transfusion for prevention of bleeding in patients with haematological disorders after chemotherapy and stem cell transplantation, Cochrane Database of Systematic Reviews 2012 16(5). http://www.ncbi.nlm.nih.gov/pubmed/22592695
-
125. Murphy S, Litwin S, Herring LM, Koch P, Remischovsky J, Donaldson MH, et al. Indications for platelet transfusion in children with acute leukemia, Am J Hematol 1982; 12(4):347-356. http://www.ncbi.nlm.nih.gov/pubmed/6981349
-
126. Roy AJ, Jaffe N and Djerassi I. Prophylactic platelet transfusions in children with acute leukemia: a dose response study, Transfusion 1973; 13(5):283-290. http://www.ncbi.nlm.nih.gov/pubmed/4750180
-
127. Kaufman RM, Djulbegovic B, Gernsheimer T, Kleinman S, Tinmouth AT, Capocelli KE, et al. Platelet transfusion: a clinical practice guideline from the AABB, Ann Intern Med 2015; 162(3):205-213. http://www.ncbi.nlm.nih.gov/pubmed/25383671
-
128. Nahirniak S, Slichter SJ, Tanael S, Rebulla P, Pavenski K, Vassallo R, et al. Guidance on platelet transfusion for patients with hypoproliferative thrombocytopenia, Transfus Med Rev 2015; 29(1):3-13. http://www.ncbi.nlm.nih.gov/pubmed/25537844
-
129. Lee JW, Yoo YC, Park HK, Bang SO, Lee KY and Bai SJ. Fresh frozen plasma in pump priming for congenital heart surgery: Evaluation of effects on postoperative coagulation profiles using a fibrinogen assay and rotational thromboelastometry, Yonsei Medical Journal 2013 54(3):752-762. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3635629/pdf/ymj-54-752.pdf
-
130. McCall MM, Blackwell MM, Smyre JT, Sistino JJ, Acsell JR, Dorman BH, et al. Fresh frozen plasma in the pediatric pump prime: A prospective, randomized trial, Annals of Thoracic Surgery 2004; 77(3):983-987. http://www.annalsthoracicsurgery.org/article/S0003-4975(03)01873-3/pdf
-
131. Oliver, Jr., Beynen FM, Nuttall GA, Schroeder DR, Ereth MH, Dearani JA, et al. Blood loss in infants and children for open heart operations: Albumin 5% versus fresh-frozen plasma in the prime, Annals of Thoracic Surgery 2003, 75(5):1506-1512. http://www.annalsthoracicsurgery.org/article/S0003-4975(02)04991-3/pdf
-
132. British Committee for Standards in Haematology BTTF. Guidelines for the use of platelet transfusions, Br J Haematol 2003; 122(1):10-23.
-
133. Lunde J, Stensballe J, Wikkelso A, Johansen M and Afshari A. Fibrinogen concentrate for bleeding–a systematic review, Acta Anaesthesiol Scand 2014; 58(9):1061-1074. http://www.ncbi.nlm.nih.gov/pubmed/25059813
-
134. Galas FRBG, de Almeida JP, Fukushima JT, Vincent JL, Osawa EA, Zeferino S, et al. Hemostatic effects of fibrinogen concentrate compared with cryoprecipitate in children after cardiac surgery: A randomized pilot trial, Journal of Thoracic and Cardiovascular Surgery. 2014. http://dx.doi.org/10.1016/j.jtcvs.2014.04.029
-
135. Church GD, Matthay MA, Liu K, Milet M and Flori HR. Blood product transfusions and clinical outcomes in pediatric patients with acute lung injury, Pediatric Critical Care Medicine 2009; 10(3): 297-302. http://www.ncbi.nlm.nih.gov/pubmed/19307809
-
136. Karam O, Lacroix J, Robitaille N, Rimensberger PC and Tucci M. Association between plasma transfusions and clinical outcome in critically ill children: A prospective observational study, Vox Sanguinis 2013; 104(4):342-349. http://onlinelibrary.wiley.com/doi/10.1111/vox.12009/abstract
-
137. Airey RJ, Farrar D and Duley L (2010). Alternative positions for the baby at birth before clamping the umbilical cord, Cochrane database of systematic reviews (10):CD007555. http://www.ncbi.nlm.nih.gov/pubmed/20927760
-
138. Vain NE, Satragno DS, Gorenstein AN, Gordillo JE, Berazategui JP, Alda MG, et al. Effect of gravity on volume of placental transfusion: a multicentre, randomised, non-inferiority trial, Lancet 2014; 384(9939):235-240. http://www.ncbi.nlm.nih.gov/pubmed/24746755
-
139. Backes CH, Rivera BK, Haque U, Bridge JA, Smith CV, Hutchon DJR, et al. Placental transfusion strategies in very preterm neonates: A systematic review and meta-analysis, Obstetrics and Gynecology 2014, 124(1):47-56. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L53180434
-
140. McCall MM, Blackwell MM, Smyre JT, Sistino JJ, Acsell JR, Dorman BH, et al. Fresh frozen plasma in the pediatric pump prime: A prospective, randomized trial, Annals of Thoracic Surgery 2004; 77(3):983-987. http://www.annalsthoracicsurgery.org/article/S0003-4975(03)01873-3/pdf
-
141. Chicella MF and Krueger KP. Prospective randomized double-blind placebo controlled trial of recombinant human erythropoietin administration to reduce blood transfusions in anemic pediatric intensive care patients, The Journal of Pediatric Pharmacology and Therapeutics 2006; 11(2):101-106. http://www.jppt.org/doi/abs/10.5863/1551-6776-11.2.101
-
142. Ghavam S, Batra D, Mercer J, Kugelman A, Hosono S, Oh W, et al. Effects of placental transfusion in extremely low birthweight infants: Meta-analysis of long- and short-term outcomes, Transfusion 2013; 54(4):1192-1198. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L52863259
-
143. Mathew JL. Timing of umbilical cord clamping in term and preterm deliveries and infant and maternal outcomes: A systematic review of randomized controlled trials, Indian Pediatrics 2011; 48(2):123-129. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L361595745
-
144. Rabe H, Diaz-Rossello JL, Duley L and Dowswell T (2012). Effect of timing of umbilical cord clamping and other strategies to influence placental transfusion at preterm birth on maternal and infant outcomes, Cochrane database of systematic reviews (Online) 8:CD003248. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L365721914
-
145. Alan S, Arsan S, Okulu E, Akin IM, Kilic A, Taskin S, et al. Effects of umbilical cord milking on the need for packed red blood cell transfusions and early neonatal hemodynamic adaptation in preterm infants born (less-than or equal to)1500 g: A prospective, randomized, controlled trial, J Pediatr Hematol Oncol. 2014. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L53054956
-
146. Katheria AC, Leone TA, Woelkers D, Garey DM, Rich W and Finer NN. The effects of umbilical cord milking on hemodynamics and neonatal outcomes in premature neonates, J Pediatr 2014; 164(5):1045-1050.e1041. http://www.jpeds.com/article/S0022-3476(14)00030-4/abstract
-
147. Bowen JR, Patterson JA, Roberts CL, Isbister JP, Irving DO and Ford JB. Red cell and platelet transfusions in neonates: a population-based study, Arch Dis Child Fetal Neonatal Ed 2015; 100(5):F11-415. http://www.ncbi.nlm.nih.gov/pubmed/25977265
-
148. Hammerman C, Vreman HJ, Kaplan M and Stevenson DK. Intravenous immune globulin in neonatal immune hemolytic disease: does it reduce hemolysis?, Acta Paediatr 1996; 85(11):1351-1353. http://www.ncbi.nlm.nih.gov/pubmed/8955465
-
149. Louis D, More K, Oberoi S and Shah PS. Intravenous immunoglobulin in isoimmune haemolytic disease of newborn: An updated systematic review and meta-analysis, Archives of Disease in Childhood: Fetal and Neonatal Edition. 2014. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L53004290
-
150. Chitty HE, Ziegler N, Savoia H, Doyle LW and Fox LM. Neonatal exchange transfusions in the 21st century: a single hospital study, J Paediatr Child Health 2013; 49(10):825-832. http://www.ncbi.nlm.nih.gov/pubmed/23834341
-
151. Liley HG, Gardener G, Lopriore E and Smits-Wintjens V (2015). Immune Hemolytic Disease, In Orkin SH, Nathan DG, et al. (eds.), Nathan and Oski’s Hematology and Oncology of Infancy and Childhood, 8th Edition, Elsevier.
-
152. Caputo M, Patel N, Angelini GD, Siena P, Stoica S, Parry AJ, et al. Effect of normothermic cardiopulmonary bypass on renal injury in pediatric cardiac surgery: a randomized controlled trial, J Thorac Cardiovasc Surg 2011, 142:1114-1121, 1121. http://www.jtcvsonline.org/article/S0022-5223(11)00848-8/pdf
-
153. Precious DS, Splinter W and Bosco D. Induced hypotensive anesthesia for adolescent orthognathic surgery patients, Journal of Oral and Maxillofacial Surgery 1996; 54(6):680-683, discussion 683-684. http://www.joms.org/article/S0278-2391(96)90679-5/abstract
-
154. National Blood Authority (NBA) (2013). National Patient Blood Management Guidelines Implementation Strategy 2013–17, NBA, Canberra, Australia.
-
155. Friesen RH, Perryman KM, Weigers KR, Mitchell MB and et al. A trial of fresh autologous whole blood to treat dilutional coagulopathy following cardiopulmonary bypass in infants, 2006; 16:429-435.
-
156. Hans P, Collin V, Bonhomme V, Damas F, Born JD and Lamy M. Evaluation of acute normovolemic hemodilution for surgical repair of craniosynostosis, Journal of Neurosurgical Anesthesiology 2000; 12(1):33-36.
-
157. Lisander B, Jonsson R and Nordwall A. Combination of blood-saving methods decreases homologous blood requirements in scoliosis surgery, Anaesthesia and Intensive Care 1996; 24(5): 555-558.
-
158. Cholette JM, Powers KS, Alfieris GM, Angona R, Henrichs KF, Masel D, et al. Transfusion of cell saver salvaged blood in neonates and infants undergoing open heart surgery significantly reduces GR and coagulant product transfusions and donor exposures: results of a prospective, randomized, clinical trial, Pediatric Critical Care Medicine 2013; 14(2):137-147. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3671922/pdf/nihms463601.pdf
-
159. Ye L, Lin R, Fan Y, Yang L, Hu J and Shu Q. Effects of circuit residual volume salvage reinfusion on the postoperative clinical outcome for pediatric patients undergoing cardiac surgery, Pediatric Cardiology 2013; 34(5):1088-1093. http://link.springer.com/article/10.1007%2Fs00246-012-0606-z
-
160. Nakayama Y, Nakajima Y, Tanaka KA, Sessler DI, Maeda S, Iida J, et al. Thromboelastometry-guided intraoperative haemostatic management reduces bleeding and red cell transfusion after paediatric cardiac surgery, Br J Anaesth 2015; 114(1):91-102. http://www.ncbi.nlm.nih.gov/pubmed/25303988
-
161. Arnold DM, Fergusson DA, Chan AKC, Cook RJ, Fraser GA, Lim W, et al. Avoiding transfusions in children undergoing cardiac surgery: A meta-analysis of randomized trials of aprotinin, Anesthesia and Analgesia 2006; 102(3):731-737. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L43306387
-
162. Faraoni D and Goobie SM. The efficacy of antifibrinolytic drugs in children undergoing noncardiac surgery: A systematic review of the literature, Anesthesia and Analgesia 2014; 118(3): 628-636. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L372489518
-
163. Ker K, Beecher D and Roberts I (2013). Topical application of tranexamic acid for the reduction of bleeding, Cochrane database of systematic reviews.
-
164. Schouten ES, Van De Pol AC, Schouten ANJ, Turner NM, Jansen NJG and Bollen CW. The effect of aprotinin, tranexamic acid, and aminocaproic acid on blood loss and use of blood products in major pediatric surgery: A meta-analysis, Pediatric Critical Care Medicine 2009; 10(2): 182-190. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L355297646
-
165. Song G, Yang P, Zhu S, Luo E, Feng G, Hu J, et al. Tranexamic acid reducing blood transfusion in children undergoing craniosynostosis surgery, Journal of Craniofacial Surgery 2013; 24(1):299-303. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L368259498
-
166. Tzortzopoulou A, Cepeda MS, Schumann R and Carr DB (2008). Antifibrinolytic agents for reducing blood loss in scoliosis surgery in children, Cochrane database of systematic reviews.
-
167. Badeaux J and Hawley D. A systematic review of the effectiveness of intravenous tranexamic acid administration in managing perioperative blood loss in patients undergoing spine surgery, J Perianesth Nurs 2014; 29(6):459-465. http://www.ncbi.nlm.nih.gov/pubmed/25458625
-
168. Basta MN, Stricker PA and Taylor JA. A systematic review of the use of antifibrinolytic agents in pediatric surgery and implications for craniofacial use, Pediatr Surg Int 2012; 28(11): 1059-1069. http://www.ncbi.nlm.nih.gov/pubmed/22940882
-
169. Aggarwal V, Kapoor PM, Choudhury M, Kiran U and Chowdhury U. Utility of sonoclot analysis and tranexamic acid in tetralogy of Fallot patients undergoing intracardiac repair, Ann Card Anaesth 2012; 15:26-31.
-
170. Coniff RF, Ceithaml EL, Pourmojhadam K, D’Errico CC, Dietrich W and Greeley WJ. Bayer 022 compassionate-use pediatric study, Annals of Thoracic Surgery 1998; 65(6 SUPPL.):S31-S34.http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L28308473
-
171. Ferreira CA, de Andrade Vicente WV, Evora PRB, Rodrigues AJ, Klamt JG, de Carvalho Panzeli Carlotti AP, et al. Assessment of aprotinin in the reduction of inflammatory systemic response in children undergoing surgery with cardiopulmonary bypass, Brazilian Journal of Cardiovascular Surgery 2010; 25(1):85-98. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L359111284
-
172. Flaujac C, Pouard P, Boutouyrie P, Emmerich J, Bachelot-Loza C and Lasne D. Platelet dysfunction after normothermic cardiopulmonary bypass in children: Effect of high-dose aprotinin, Thrombosis and Haemostasis 2007; 98(2):385-391. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L47250242
-
173. Sarupria A, Makhija N, Lakshmy R and Kiran U. Comparison of different doses of (epsilon)- aminocaproic acid in children for tetralogy of fallot surgery: Clinical efficacy and safety, Journal of Cardiothoracic and Vascular Anesthesia 2013; 27(1):23-29. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L52215993
-
174. Singh R, Manimozhi V, Nagaraj G, Vasanth K, Sanjay KB, John C, et al. Aprotinin for open cardiac surgery in cyanotic heart disease, Asian Cardiovascular and Thoracic Annals 2001; 9(2):101-104. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L32618900
-
175. Vacharaksa K, Prakanrattana U, Suksompong S and Chumpathong S. Tranexamic acid as a means of reducing the need for blood and blood component therapy in children undergoing open heart surgery for congenital cyanotic heart disease, Journal of the Medical Association of Thailand 2002; 85(SUPPL. 3):S904-S909. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L36025031
-
176. Thompson GH, Florentino-Pineda I and Poe-Kochert C. The Role of Amicar in Decreasing Perioperative Blood Loss in Idiopathic Scoliosis Spine 2005; 30:S94-S99.
-
177. Verma K, Errico T, Diefenbach C, Hoelscher C, Peters A, Dryer J, et al. The relative efficacy of antifibrinolytics in adolescent idiopathic scoliosis: A prospective randomized trial, Journal of Bone and Joint Surgery American 2014; Volume 96:e80-e80.
-
178. Ahmed Z, Stricker L, Rozzelle A and Zestos M. Aprotinin and transfusion requirements in pediatric craniofacial surgery, Paediatr Anaesth 2014; 24:141-145.
-
179. D’Errico CC, Munro HM, Buchman SR, Wagner D and Muraszko KM. Efficacy of aprotinin in children undergoing craniofacial surgery, J Neurosurg 2003; 99:287-290.
-
180. Eldaba AA, Amr YM and Albirmawy OA. Effects of tranexamic acid during endoscopic sinsus surgery in children, Saudi Journal of Anaesthesia 2013; 7:229-233. http://www.saudija.org/article.asp?issn=1658-354X;year=2013;volume=7;issue=3;spage=229;ep age=233;aulast=Eldaba
-
181. Florentino-Pineda I, Thompson GH, Poe-Kochert C, Huang RP, Haber LL and Blakemore LC. The effect of Amicar in perioperative blood loss in idiopathic scoliosis. The results of a prospective, randomized double-blind study, Spine 2004; 29:233-238.
-
182. Khoshhal K, Mukhtar I, Clark P, Jarvis J, Letts M and Splinter W. Efficacy of aprotinin in reducing blood loss in spinal fusion for idiopathic scoliosis, J Paediatr Orthop 2003; 23:661-664.
-
183. Neilipovitz D, Murto K, Hall L, Barrowman N and Splinter W. A randomized trial of tranexamic acid to reduce blood transfusion for scoliosis surgery, Anesth Analg 2001; 93:82-87.
-
184. Sethna NF, Zurakowski D, Brustowicz M, Bacsik J, Sullivan L and Shapiro F. Tranexamic acid reduces intraoperative blood loss in pediatric patients undergoing scoliosis surgery, Anesthesiology 2005; 102:727-732.
-
185. Dadure C, Sauter M, Bringuier S, Bigorre M, Raux O, Rochette A, et al. Intraoperative tranexamic acid reduces blood transfusion in children undergoing craniosynostosis surgery: a randomized double-blind study, Anesthesiology 2011; 114:856-861. http://anesthesiology.pubs.asahq.org/data/Journals/JASA/931106/0000542-201104000- 00020.pdf
-
186. Goobie SM, Meier PM, Pereira LM, McGowan FX, Prescilla RP, Scharp LA, et al. Efficacy of tranexamic acid in pediatric craniosynostosis surgery: a double-blind, placebo-controlled trial, Anesthesiology 2011; 114:862-871. http://anesthesiology.pubs.asahq.org/data/Journals/JASA/931106/0000542-201104000-00021.pdf
-
187. Maugans TA, Martin D, Taylor J, Salisbury S and Istaphanous G. Comparative analysis of tranexamic acid use in minimally invasive versus open craniosynostosis procedures, Journal of Craniofacial Surgery 2011; 22(5):1772-1778. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L362692909
-
188. Albirmawy OA, Saafan ME, Shehata EM, Basuni AS and Eldaba AA. Topical application of tranexamic acid after adenoidectomy: A double-blind, prospective, randomized, controlled study, International Journal of Pediatric Otorhinolaryngology 2013; 77:1139-1142. http://www.ijporlonline.com/article/S0165-5876(13)00180-8/abstract
-
189. Cole JW, Murray DJ, Snider RJ, Bassett GS, Bridwell KH and Lenke LG. Aprotinin reduces blood loss during spinal surgery in children, 2003; 28:2482-2485.
-
190. Faraoni D, Willems A, Melot C, De Hert S and Van der Linden P. Efficacy of tranexamic acid in paediatric cardiac surgery: A systematic review and meta-analysis, European Journal of Cardio-Thoracic Surgery 2012; 42(5):781-786. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L368247390
-
191. Chauhan S, Das SN, Bisoi A, Kale S and Kiran U. Comparison of Epsilon Aminocaproic Acid and Tranexamic Acid in Pediatric Cardiac Surgery, Journal of Cardiothoracic and Vascular Anesthesia 2004a; 18(2):141-143. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L38506857
-
192. Brum MR, Miura MS, Castro SF, Machado GM, Lima LH and Lubianca-Neto JF. Tranexamic acid in adenotonsillectomy in children: a double-blind randomized clinical trial, International Journal of Pediatric Otorhinolaryngology 2012; 76:1401-1405. http://www.ijporlonline.com/article/S0165-5876(12)00292-3/abstract
-
193. Pasquali SK, Li JS, He X, Jacobs ML, O’Brien SM, Hall M, et al. Comparative analysis of antifibrinolytic medications in pediatric heart surgery, J Thorac Cardiovasc Surg 2012; 143(3):550-557. http://www.ncbi.nlm.nih.gov/pubmed/22264414
-
194. Goobie SM, Meier PM, Sethna NF, Soriano SG, Zurakowski D, Samant S, et al. Population pharmacokinetics of tranexamic acid in paediatric patients undergoing craniosynostosis surgery, Clin Pharmacokinet 2013; 52(4):267-276. http://www.ncbi.nlm.nih.gov/pubmed/23371895
-
195. Wesley MC, Pereira LM, Scharp LA, Emani SM, McGowan FX, Jr. and DiNardo JA. Pharmacokinetics of tranexamic acid in neonates, infants, and children undergoing cardiac surgery with cardiopulmonary bypass, Anesthesiology 2015; 122(4):746–758. http://www.ncbi.nlm.nih.gov/pubmed/25585004
-
196. Luban NLC (2012). Transfusion of blood and blood products, In MacDonald M, Ramasethu J, et al. (eds.), Atlas of procedures in neonatology, Fifth edition Wolters Kluwer/Lippincott Williams & Wilkins.
-
197. Davies P, Robertson S, Hegde S, Greenwood R, Massey E and Davis P (2007). Calculating the required transfusion volume in children, Transfusion 2007; 47(2):212-216. http://www.ncbi.nlm.nih.gov/pubmed/17302766
-
198. Simpson E, Lin Y, Stanworth S, Birchall J, Doree C and Hyde C (2012). Recombinant factor VIIa for the prevention and treatment of bleeding in patients without haemophilia, Cochrane database of systematic reviews.
-
199. Ekert H, Brizard C, Eyers R, Cochrane A and Henning R. Elective administration in infants of low-dose recombinant activated factor VII (rFVIIa) in cardiopulmonary bypass surgery for congenital heart disease does not shorten time to chest closure or reduce blood loss and need for transfusions, Blood Coagulation and Fibrinolysis 2006; 17(5):389-395. http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L43941581
-
200. Mozol K, Haponiuk I, Byszewski A and Maruszewski B. Cost-effectiveness of mini-circuit cardiopulmonary bypass in newborns and infants undergoing open heart surgery, Kardiologia. Polska 2008; 66:925-931.
-
201. Hess JR and Greenwalt TG. Storage of red blood cells: new approaches, Transfus Med Rev 2002; 16(4):283-295. http://www.ncbi.nlm.nih.gov/pubmed/12415514
-
202. Triulzi DJ and Yazer MH. Clinical studies of the effect of blood storage on patient outcomes, Transfus Apher Sci 2010; 43(1):95-106. http://www.ncbi.nlm.nih.gov/pubmed/20656558
-
203. Gibson BE, Todd A, Roberts I, Pamphilon D, Rodeck C, Bolton-Maggs P, et al. Transfusion guidelines for neonates and older children, Br J Haematol 2004; 124(4):433-453. http://www.ncbi.nlm.nih.gov/pubmed/14984493
-
204. Kennedy MS (2011). Perinatal issues in transfusion practice, In Roback JD, Grossman BJ, et al. (eds.), Technical Manual, AABB, Bethesda, MD, 631-644.
-
205. Strauss RG. GR storage and avoiding hyperkalemia from transfusions to neonates & infants, Transfusion 2010; 50(9):1862-1865. http://www.ncbi.nlm.nih.gov/pubmed/21552366
-
206. The Royal Children’s Hospital (RCH), Exchange transfusion: Neonatal, RCH, Melbourne. http://www.rch.org.au/uploadedFiles/Main/Content/neonatal_rch/EXCHANGE_TRANSFUSION.pdf
-
207. Ramasethu J (2012). Exchange transfusion, In MacDonald M, Ramasethu J, et al. (eds.), Atlas of procedures in neonatology, Fifth edition Wolters Kluwer/Lippincott Williams & Wilkins.
-
208. UK Blood Transfusion & Tissue Transplantation Services (2013). Guidelines for the blood tranfusion services in the United Kingdom, The Stationary Office, London.
-
209. Australian & New Zealand Society of Blood Transfusion Inc (ANZSBT) (2007). Guidelines for pretransfusion laboratory practice, 3rd Edition, ANZSBT. http://www.anzsbt.org.au/publications/documents/PLP_Guidelines_Mar07.pdf
-
210. Ranucci M, Carlucci C, Isgro G, Boncilli A, De Benedetti D, De la Torre T, et al. Duration of red blood cell storage and outcomes in pediatric cardiac surgery: an association found for pump prime blood, Crit Care 2009; 13(6):R207. http://www.ncbi.nlm.nih.gov/pubmed/20025760
-
211. Fergusson DA, Hebert P, Hogan DL, LeBel L, Rouvinez-Bouali N, Smyth JA, et al. Effect of fresh red blood cell transfusions on clinical outcomes in premature, very low-birth-weight infants: the ARIPI randomized trial, JAMA 2012; 308(14):1443-1451.n http://www.ncbi.nlm.nih.gov/pubmed/23045213
-
212. Gauvin F, Spinella PC, Lacroix J, Choker G, Ducruet T, Karam O, et al. Association between length of storage of transfused red blood cells and multiple organ dysfunction syndrome in pediatric intensive care patients, Transfusion 2010; 50(9):1902-1913. http://www.ncbi.nlm.nih.gov/pubmed/20456697
-
213. Karam O, Tucci M, Bateman ST, Ducruet T, Spinella PC, Randolph AG, et al. Association between length of storage of red blood cell units and outcome of critically ill children: a prospective observational study, Crit Care 2010; 14(2):R57. http://www.ncbi.nlm.nih.gov/pubmed/20377853
-
214. Australian & New Zealand Society of Blood Transfusion Inc (ANZSBT). Guidelines for blood grouping & antibody screening in the antenatal & perinatal setting, 3rd Edition, ANZSBT. http://www.anzsbt.org.au/publications/documents/Antenatal_Guidelines_Mar07.pdf
-
215. Wamelen DJ, Klumper FJ, de Haas M, Meerman RH, van Kamp IL and Oepkes D. Obstetric history and antibody titer in estimating severity of Kell alloimmunization in pregnancy, Obstet Gynecol 2007; 109(5):1093-1098. http://www.ncbi.nlm.nih.gov/pubmed/17470588
-
216. Norfolk D (2013). Handbook of transfusion medicine (5th edition), United Kingdom Blood Services, The Stationery Office, London. http://www.transfusionguidelines.org.uk/transfusion-handbook
-
217. Treleaven J, Gennery A, Marsh J, Norfolk D, Page L, Parker A, et al. Guidelines on the use of irradiated blood components prepared by the British Committee for Standards in Haematology blood transfusion task force, Br J Haematol 2011; 152(1):35-51.
-
218. Australian & New Zealand Society of Blood Transfusion (ANZSBT) (2011). Prevention of transfusion-associated graft-versus-host disease (TA-GVHD), ANZBST. http://www.anzsbt.org.au/publications/index.cfm#societyg
-
219. Vamvakas EC. Is white blood cell reduction equivalent to antibody screening in preventing transmission of cytomegalovirus by transfusion? A review of the literature and meta-analysis, Transfus Med Rev 2005; 19(3):181-199. http://www.tmreviews.com/article/S0887-7963(05)00012-X/abstract
-
220. Preiksaitis JK. The cytomegalovirus-”safe” blood product: is leukoreduction equivalent to antibody screening?, Transfus Med Rev 2000; 14(2):112-136. http://www.tmreviews.com/article/S0887-7963(00)80003-6/abstract
-
221. Drew WL and Roback JD. Prevention of transfusion-transmitted cytomegalovirus: reactivation of the debate?, Transfusion 2007; 47(11):1955-1958. http://onlinelibrary.wiley.com/doi/10.1111/j.1537-2995.2007.01494.x/abstract
-
222. Seed CR, Wong J, Polizzotto MN, Faddy H, Keller AJ and Pink J. The residual risk of transfusion-transmitted cytomegalovirus infection associated with leucodepleted blood components, Vox Sang 2015; 109(1):11-17. http://www.ncbi.nlm.nih.gov/pubmed/25854287
-
223. Roback JD, Conlan M, Drew WL, Ljungman P, Nichols WG and Preiksaitis JK. The role of photochemical treatment with amotosalen and UV-A light in the prevention of transfusion-transmitted cytomegalovirus infections, Transfus Med Rev 2006; 20(1):45-56. http://www.tmreviews.com/article/S0887-7963(05)00081-7/abstract
-
224. Canadian Blood Services (2011). CMV seronegative, irradiated and washed blood components, Clinical guide to transfusion. http://www.transfusionmedicine.ca/resources/clinical-guide-transfusion
-
225. American Association of Blood Banks (1997). Statement of the American Association of Blood Banks Before the Blood Products Advisory Committee on the Effect of Leukoreduction on CMV Transmission Through Blood Transfusion. AABB Bulletin #97-2.
-
226. Advisory Committee on the Safety of Blood TaOS (2012). Cytomegalovirus tested blood components: Position Statement. SaBTO report of the Cytomegalovirus Steering Group, Department of Health. https://www.gov.uk/government/uploads/system/uploads/attachment_data/file/215125/ dh_133086.pdf
-
227. Thiele T, Kruger W, Zimmermann K, Ittermann T, Wessel A, Steinmetz I, et al. Transmission of cytomegalovirus (CMV) infection by leukoreduced blood products not tested for CMV antibodies: a single-center prospective study in high-risk patients undergoing allogeneic hematopoietic stem cell transplantation (CME), Transfusion 2011; 51(12):2620-2626. http://www.ncbi.nlm.nih.gov/pubmed/21645009
-
228. Nash T, Hoffmann S, Butch S, Davenport R and Cooling L. Safety of leukoreduced, cytomegalovirus (CMV)-untested components in CMV-negative allogeneic human progenitor cell transplant recipients, Transfusion 2012; 52(10):2270-2272. http://onlinelibrary.wiley.com/doi/10.1111/j.1537-2995.2012.03739.x/abstract
-
229. Curtis BR and McFarland JG. Human platelet antigens – 2013, Vox Sang 2014; 106(2):93-102. http://www.ncbi.nlm.nih.gov/pubmed/24102564
-
230. Mueller-Eckhardt C KV, Grubert A et al. 348 cases of suspected neonatal alloimmune thrombocytopenia, The Lancet 1989; 1:363-366.
-
231. Davoren A CBR, Aster R.H, McFarland J.G. Human platelet antigen-specific alloantibodies implicated in 1162 cases of neonatal alloimmune thrombocytopenia, Transfusion 2004; 44:1220-1225.
-
232. Bennett JA, Palmer LJ, Musk AW and Erber WN. Gene frequencies of human platelet antigens 1-5 in indigenous Australians in Western Australia, Transfus Med 2002; 12(3):199-203. http://www.ncbi.nlm.nih.gov/pubmed/12071877
-
233. Sainio S, Jarvenpaa AL, Renlund M, Riikonen S, Teramo K and Kekomaki R. Thrombocytopenia in term infants: a population-based study, Obstet Gynecol 2000; 95(3):441-446. http://www.ncbi.nlm.nih.gov/pubmed/10711560
-
234. Spencer JA and Burrows RF. Feto-maternal alloimmune thrombocytopenia: a literature review and statistical analysis, Aust N Z J Obstet Gynaecol 2001; 41(1):45-55. http://www.ncbi.nlm.nih.gov/pubmed/11284646
-
235. Risson DC, Davies MW and Williams BA. Review of neonatal alloimmune thrombocytopenia, Journal of Paediatrics and Child Health 2012; 48:816-822.
-
236. Bakchoul T BD, Heckmann M et al. Management of infants born with severe neonatal alloimmune thrombocytopenia: the role of platelet transfusions and intravenous immunoglobulin, Transfusion 2014, 54(3):640-645.
-
237. Kiefel V BD, Kroll H et al. Antigen-positive platelet transfusion in neonatal alloimmune thrombocytopenia (NAIT), Blood 2006; 107:3761-3763.
-
238. Win N, Ouwehand WH and Hurd C. Provision of platelets for severe neonatal thrombocytopenia, Br J Haematol 1997; 97:927-940.
-
239. Stroncek DF and Rebulla P (). Platelet transfusions, Lancet 2007; 370(9585):427-438. http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(07)61198-2/abstract
-
240. Williamson LM. Leucocyte depletion of the blood supply – how will patients benefit?, Br J Haematol 2000; 110(2):256-272.
-
241. Bolton-Maggs PH, Chalmers EA, Collins PW, Harrison P, Kitchen S, Liesner RJ, et al. A review of inherited platelet disorders with guidelines for their management on behalf of the UKHCDO, Br J Haematol 2006; 135(5):603-633.
-
242. Schlegel N, Bardet V, Kenet G, Muntean W, Zieger B, Nowak-Gottl U, et al. Diagnostic and therapeutic considerations on inherited platelet disorders in neonates and children, Klinische Padiatrie 2010; 222(3):209-214. https://www.thieme-connect.com/DOI/DOI?10.1055/s-0030-1249065
-
243. Blumberg N, Heal JM and Rowe JM. A randomized trial of washed red blood cell and platelet transfusions in adult acute leukemia [ISECAN76536440], BMC blood disorders 2004; 4(1):6. http://www.ncbi.nlm.nih.gov/pubmed/15588315
-
244. National Health and Medical Research Council (NHMRC) (2011). Procedures and requirements for meeting the 2011 NHMRC standard for clinical practice guidelines, NHMRC, Canberra, Australia. http://www.nhmrc.gov.au/guidelines/publications/cp133-and-cp133a
-
245. Blumberg N, Heal JM, Gettings KF, Phipps RP, Masel D, Refaai MA, et al. An association between decreased cardiopulmonary complications (transfusion-related acute lung injury and transfusion-associated circulatory overload) and implementation of universal leukoreduction of blood transfusions, Transfusion 2010, 50(12):2738-2744. http://www.ncbi.nlm.nih.gov/pubmed/20561296
-
246. Belizaire RM, Makley AT, Campion EM, Sonnier DI, Goodman MD, Dorlac WC, et al. Resuscitation with washed aged packed red blood cell units decreases the proinflammatory response in mice after hemorrhage, J Trauma Acute Care Surg 2012; 73(2 Suppl 1):S128-133. http://www.ncbi.nlm.nih.gov/pubmed/22847082
-
247. Moise K (2013). Intrauterine fetal transfusion of red blood cells, In Lockwood C & Barss V (eds.), UpToDate. http://www.uptodate.com/contents/intrauterine-fetal-transfusion-of-red-blood-cells
-
248. Cholette JM, Henrichs KF, Alfieris GM, Powers KS, Phipps R, Spinelli SL, et al. Washing red blood cells and platelets transfused in cardiac surgery reduces postoperative inflammation and number of transfusions: results of a prospective, randomized, controlled clinical trial, Pediatr Crit Care Med 2012; 13(3):290-299. http://www.ncbi.nlm.nih.gov/pubmed/21926663
-
249. Hosking MP, Beynen FM, Raimundo HS, Oliver WC, Jr. and Williamson KR. A comparison of washed red blood cells versus packed red blood cells (AS-1) for cardiopulmonary bypass prime and their effects on blood glucose concentration in children, Anesthesiology 1990; 72(6):987-990. http://www.ncbi.nlm.nih.gov/pubmed/2112346
-
250. Swindell CG, Barker TA, McGuirk SP, Jones TJ, Barron DJ, Brawn WJ, et al. Washing of irradiated red blood cells prevents hyperkalaemia during cardiopulmonary bypass in neonates and infants undergoing surgery for complex congenital heart disease, Eur J Cardiothorac Surg 2007; 31(4):659-664. http://www.ncbi.nlm.nih.gov/pubmed/17291775
-
251. Strauss RG. Data-driven blood banking practices for neonatal GR transfusions, Transfusion 2000; 40(12):1528-1540. http://www.ncbi.nlm.nih.gov/pubmed/11134575
-
252. van Kamp IL, Klumper FJCM, Meerman RH, Oepkes D, Scherjon SA and Kanhai HH. Treatment of fetal anemia due to red-cell alloimmunization with intrauterine transfusions in the Netherlands, 1988-1999, Acta Obstetricia et Gynecologica Scandinavica 2004; 83(8):731-737. http://onlinelibrary.wiley.com/doi/10.1111/j.0001-6349.2004.00394.x/abstract
-
253. Somerset DA, Moore A, Whittle MJ, Martin W and Kilby MD. An audit of outcome in intravascular transfusions using the intrahepatic portion of the fetal umbilical vein compared to cordocentesis, Fetal Diagnosis and Therapy 2006; 21(3):272-276.
-
254. Mari G, Deter RL, Carpenter RL, Rahman F, Zimmerman R, Moise KJ, Jr., et al. Noninvasive diagnosis by Doppler ultrasonography of fetal anemia due to maternal red-cell alloimmunization. Collaborative Group for Doppler Assessment of the Blood Velocity in Anemic Fetuses, N Engl J Med 2000; 342(1):9-14. http://www.ncbi.nlm.nih.gov/pubmed/10620643
-
255. Scheier M, Hernandez-Andrade E, Fonseca EB and Nicolaides KH. Prediction of severe fetal anemia in red blood cell alloimmunization after previous intrauterine transfusions, Am J Obstet Gynecol 2006; 195(6):1550-1556. http://www.ajog.org/article/S0002-9378(06)00447-9/abstract
-
256. Detti L, Oz U, Guney I, Ferguson JE, Bahado-Singh RO, Mari G, et al. Doppler ultrasound velocimetry for timing the second intrauterine transfusion in fetuses with anemia from red cell alloimmunization, Am J Obstet Gynecol 2001; 185(5):1048-1051. http://www.ncbi.nlm.nih.gov/pubmed/11717631
-
257. Wong KS, Connan K, Rowlands S, Kornman LH and Savoia HF (2013). Antenatal immunoglobulin for fetal red blood cell alloimmunization, Cochrane Database Syst Rev 5:CD008267. http://www.ncbi.nlm.nih.gov/pubmed/23728672
-
258. Van Kamp IL, Klumper FJCM, Oepkes D, Meerman RH, Scherjon SA, Vandenbussche FP, et al. Complications of intrauterine intravascular transfusion for fetal anemia due to maternal red-cell alloimmunization, Am J Obstet Gynecol 2005; 192(1):171-177.
-
259. Canlorbe G, Mace G, Cortey A, Cynober E, Castaigne V, Larsen M, et al. Management of very early fetal anemia resulting from red-cell alloimmunization before 20 weeks of gestation, Obstetrics and Gynecology 2011; 118(6):1323-1329.
-
260. Bateman ST, Lacroix J, Boven K, Forbes P, Barton R, Thomas NJ, et al. Anemia, blood loss, and blood transfusions in North American children in the intensive care unit, Am J Respir Crit Care Med 2008; 178(1):26-33. http://www.ncbi.nlm.nih.gov/pubmed/18420962
-
261. Bednarek FJ, Weisberger S, Richardson DK, Frantz ID, 3rd, Shah B and Rubin PL. Variations in blood transfusions among newborn intensive care units. SNAP II Study Group, J Pediatr 1998; 133(5):601-607. http://www.ncbi.nlm.nih.gov/pubmed/9821414
-
262. Valentine SL and Bateman ST. Identifying factors to minimize phlebotomy-induced blood loss in the pediatric intensive care unit, Pediatr Crit Care Med 2012; 13(1):22-27. http://www.ncbi.nlm.nih.gov/pubmed/21499175
-
263. Lin JC, Strauss RG, Kulhavy JC, Johnson KJ, Zimmerman MB, Cress GA, et al. Phlebotomy overdraw in the neonatal intensive care nursery, Pediatrics 2000; 106(2):E19. http://www.ncbi.nlm.nih.gov/pubmed/10920175
-
264. Raju TN, Stevenson DK, Higgins RD and Stark AR. Safe and effective devices and instruments for use in the neonatal intensive care units: NICHD Workshop summary, Biomed Instrum Technol 2009; 43(5):408-418. http://www.ncbi.nlm.nih.gov/pubmed/19842778
-
265. Obladen M, Sachsenweger M and Stahnke M. Blood sampling in very low birth weight infants receiving different levels of intensive care, Eur J Pediatr 1988; 147(4):399-404. http://www.ncbi.nlm.nih.gov/pubmed/3396595
-
266. Barie PS and Hydo LJ. Lessons learned: durability and progress of a program for ancillary cost reduction in surgical critical care, J Trauma 1997; 43(4):590-594; discussion 594-596. http://www.ncbi.nlm.nih.gov/pubmed/9356053
-
267. Prat G, Lefevre M, Nowak E, Tonnelier JM, Renault A, L’Her E, et al. Impact of clinical guidelines to improve appropriateness of laboratory tests and chest radiographs, Intensive Care Med 2009; 35(6):1047-1053. http://www.ncbi.nlm.nih.gov/pubmed/19221715
-
268. Roberts DE, Bell DD, Ostryzniuk T, Dobson K, Oppenheimer L, Martens D, et al. Eliminating needless testing in intensive care–an information-based team management approach, Crit Care Med 1993; 21(10):1452-1458. http://www.ncbi.nlm.nih.gov/pubmed/8403952}
-
269. Bishara N and Ohls RK. Current controversies in the management of the anemia of prematurity, Semin Perinatol 2009; 33(1):29-34. http://www.ncbi.nlm.nih.gov/pubmed/19167579
-
270. Carroll PD and Widness JA. Nonpharmacological, blood conservation techniques for preventing neonatal anemia–effective and promising strategies for reducing transfusion, Semin Perinatol 2012; 36(4):232-243. http://www.ncbi.nlm.nih.gov/pubmed/22818543
-
271. Christensen RD, Carroll PD and Josephson CD. Evidence-based advances in transfusion practice in neonatal intensive care units, Neonatology 2014; 106(3):245-253. http://www.ncbi.nlm.nih.gov/pubmed/25300949
-
272. McEvoy MT and Shander A. Anemia, bleeding, and blood transfusion in the intensive care unit: causes, risks, costs, and new strategies, Am J Crit Care 2013; 22(6 Suppl):eS1-13; quiz eS14. http://www.ncbi.nlm.nih.gov/pubmed/24186829
-
273. Shander A and Goodnough LT. Objectives and limitations of bloodless medical care, Curr Opin Hematol 2006; 13(6):462-470. http://www.ncbi.nlm.nih.gov/pubmed/17053460
-
274. Weiss M, Fischer J, Boeckmann M, Rohrer B and Baenziger O. Evaluation of a simple method for minimizing iatrogenic blood loss from discard volumes in critically ill newborns and children, Intensive Care Med 2001; 27(6):1064-1072. http://www.ncbi.nlm.nih.gov/pubmed/11497140
-
275. Page C, Retter A and Wyncoll D. Blood conservation devices in critical care: a narrative review, Ann Intensive Care 2013; 3:14. http://www.ncbi.nlm.nih.gov/pubmed/23714376
-
276. Tang M, Feng M, Chen L, Zhang J, Ji P and Luo S. Closed blood conservation device for reducing catheter-related infections in children after cardiac surgery, Crit Care Nurse 2014; 34(5):53-60; quiz 61. http://www.ncbi.nlm.nih.gov/pubmed/25274764
-
277. Billman GF, Hughes AB, Dudell GG, Waldman E, Adcock LM, Hall DM, et al. Clinical performance of an in-line, ex vivo point-of-care monitor: a multicenter study, Clin Chem 2002; 48(11):2030-2043. http://www.ncbi.nlm.nih.gov/pubmed/12406990
-
278. Widness JA, Madan A, Grindeanu LA, Zimmerman MB, Wong DK and Stevenson DK. Reduction in red blood cell transfusions among preterm infants: results of a randomized trial with an in-line blood gas and chemistry monitor, Pediatrics 2005; 115(5):1299-1306. http://www.ncbi.nlm.nih.gov/pubmed/15867038
-
279. Tran HA, Chunilal SD, Harper PL, Tran H, Wood EM, Gallus AS, et al. An update of consensus guidelines for warfarin reversal, The Medical Journal of Australia 2013; 198(4):198-199. https://www.mja.com.au/system/files/issues/tra10614_web_fm_0.pdf
-
280. Demeyere R, Gillardin S, Arnout J and Strengers PF. Comparison of fresh frozen plasma and prothrombin complex concentrate for the reversal of oral anticoagulants in patients undergoing cardiopulmonary bypass surgery: a randomized study, Vox Sanguinis 2010; 99(3):251-260. http://onlinelibrary.wiley.com/doi/10.1111/j.1423-0410.2010.01339.x/abstract
-
281. Giorni C, Ricci Z, Iodice F, Garisto C, Favia I, Polito A, et al. Use of Confidex to control perioperative bleeding in pediatric heart surgery: prospective cohort study, Pediatr Cardiol 2014; 35(2):208-214. http://www.ncbi.nlm.nih.gov/pubmed/23843105
-
282. Arnekian V, Camous J, Fattal S, Rezaiguia-Delclaux S, Nottin R and Stephan F. Use of prothrombin complex concentrate for excessive bleeding after cardiac surgery, Interactive Cardiovascular and Thoracic Surgery 2012; 15(3):382-389. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3422937/pdf/ivs224.pdf
-
283. Bobbitt L, Merriman E, Raynes J, Henderson R, Blacklock H and Chunilal S. PROTHROMBINEX((R))-VF (PTX-VF) usage for reversal of coagulopathy: prospective evaluation of thrombogenic risk, Thrombosis Research 2011; 28(6):577-582. http://www.thrombosisresearch.com/article/S0049-3848(11)00180-0/abstract
-
284. Streiff MB. Prothrombin complex concentrates for reversal of vitamin K antagonists: assessing the risks, Thrombosis and Haemostasis 2011; 106(3):389-390.
-
285. Dentali F, Marchesi C, Pierfranceschi MG, Crowther M, Garcia D, Hylek E, et al. Safety of prothrombin complex concentrates for rapid anticoagulation reversal of vitamin K antagonists. A meta-analysis, Thrombosis and Haemostasis 2011; 106(3):429-438.
-
286. Toy P, Gajic O, Bacchetti P, Looney MR, Gropper MA, Hubmayr R, et al. Transfusion-related acute lung injury: incidence and risk factors, Blood 2012; 119(7):1757-1767. http://www.bloodjournal.org/content/bloodjournal/119/7/1757.full.pdf
-
287. Alam A, Lin Y, Lima A, Hansen M and Callum JL. The prevention of transfusion-associated circulatory overload, Transfus Med Rev 2013; 27(2):105-112. http://www.tmreviews.com/article/S0887-7963(13)00005-9/abstract
-
288. Popovsky MA. Pulmonary consequences of transfusion: TRALI and TACO, Transfusion and Apheresis Science 2006; 34(3):243-244. http://www.trasci.com/article/S1473-0502(06)00054-1/abstract 289. Serious Hazards of T (2011). Annual SHOT Report.
-
290. Li G, Rachmale S, Kojicic M, Shahjehan K, Malinchoc M, Kor DJ, et al. Incidence and transfusion risk factors for transfusion-associated circulatory overload among medical intensive care unit patients, Transfusion 2011; 51(2):338-343. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3006039/pdf/nihms219753.pdf
-
291. Narick C, Triulzi DJ and Yazer MH. Transfusion-associated circulatory overload after plasma transfusion, Transfusion 2012; 52(1):160-165. http://onlinelibrary.wiley.com/doi/10.1111/j.1537-2995.2011.03247.x/abstract
-
292. Zou S, Dorsey KA, Notari EP, Foster GA, Krysztof DE, Musavi F, et al. Prevalence, incidence, and residual risk of human immunodeficiency virus and hepatitis C virus infections among United States blood donors since the introduction of nucleic acid testing, Transfusion 2010; 50(7):1495-1504. http://onlinelibrary.wiley.com/doi/10.1111/j.1537-2995.2010.02622.x/abstract
-
293. Zou S, Stramer SL, Notari EP, Kuhns MC, Krysztof D, Musavi F, et al. Current incidence and residual risk of hepatitis B infection among blood donors in the United States, Transfusion 2009; 49(8):1609-1620. http://onlinelibrary.wiley.com/doi/10.1111/j.1537-2995.2009.02195.x/abstract
-
294. Pace Napoleone C, Valori A, Crupi G, Ocello S, Santoro F, Vouhe P, et al. An observational study of CoSeal for the prevention of adhesions in pediatric cardiac surgery, Interactive Cardiovascular and Thoracic Surgery 2009; 9(6):978-982. http://icvts.oxfordjournals.org/content/9/6/978.full.pdf
-
295. Kuschel TJ, Gruszka A, Hermanns-Sachweh B, Elyakoubi J, Sachweh JS, Vazquez-Jimenez JF, et al. Prevention of postoperative pericardial adhesions with TachoSil, The Annals of Thoracic Surgery 2013; 95(1):183-188. http://www.annalsthoracicsurgery.org/article/S0003-4975(12)01889-9/pdf
-
296. Tackett SM, Sugarman R, Kreuwel HTC, Alvarez P and Nasso G. Hospital economic impact from hemostatic matrix usage in cardiac surgery, Journal of Medical Economics 2014; 17(9):670-676. http://informahealthcare.com/doi/pdfplus/10.3111/13696998.2014.928638
-
297. Baker RI, Coughlin PB, Gallus AS, Harper PL, Salem HH, Wood EM, et al. Warfarin reversal: consensus guidelines, on behalf of the Australasian Society of Thrombosis and Haemostasis, The Medical Journal of Australia 2004; 181(9):492-497. https://www.mja.com.au/system/files/issues/181_09_011104/bak10441_fm.pdf
-
298. LeMaire SA, Schmittling ZC, Coselli JS, Undar A, Deady BA, Clubb FJ, et al. BioGlue surgical adhesive impairs aortic growth and causes anastomotic strictures, The Annals of Thoracic Surgery 2002; 73(5):1500-1505, discussion 1506. http://www.annalsthoracicsurgery.org/article/S0003-4975(02)03512-9/pdf
-
299. Ortel TL, Mercer MC, Thames EH, Moore KD and Lawson JH. Immunologic impact and clinical outcomes after surgical exposure to bovine thrombin, Annals of Surgery 2001; 233(1):88-96. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1421171/pdf/20010100s00014p88.pdf
-
300. Cauchy F, Gaujoux S, Ronot M, Fuks D, Dokmak S, Sauvanet A, et al. Local venous thrombotic risk of an expanding haemostatic agent used during liver resection, World Journal of Surgery 2014; 38(9):2363-2369. http://link.springer.com/article/10.1007%2Fs00268-014-2552-9
-
301. Robicsek F. Microfibrillar collagen hemostat in cardiac surgery, J Thorac Cardiovasc Surg 2004; 127(4):1228-, author reply 1228. http://www.jtcvsonline.org/article/S0022-5223(04)00017-0/pdf
-
302. Robicsek F, Masters TN, Littman L and Born GV. The embolization of bone wax from sternotomy incisions, The Annals of Thoracic Surgery 1981; 31(4):357-359. http://www.annalsthoracicsurgery.org/article/S0003-4975(10)60967-8/pdf
-
303. Yang JC, Kim TW and Park KH. Gelfoam-induced swallowing difficulty after anterior cervical spine surgery, Korean Journal of Spine 2013; 10(2):94-96. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3941718/pdf/kjs-10-94.pdf
-
304. Vestergaard RF, Nielsen PH, Terp KA, Søballe K, Andersen G and Hasenkam JM. Effect of hemostatic material on sternal healing after cardiac surgery, The Annals of Thoracic Surgery 2014; 97(1):153-160. http://www.annalsthoracicsurgery.org/article/S0003-4975(13)01900-0/pdf
-
305. Kazui T, Washiyama N, Bashar AH, Terada H, Suzuki K, Yamashita K, et al. Role of biologic glue repair of proximal aortic dissection in the development of early and midterm redissection of the aortic root, The Annals of Thoracic Surgery 2001; 72(2):509-514. http://www.annalsthoracicsurgery.org/article/S0003-4975(01)02777-1/pdf
-
306. Ngaage DL, Edwards WD, Bell MR and Sundt TM. A cautionary note regarding long-term sequelae of biologic glue, J Thorac Cardiovasc Surg 2005; 129(4):937-938. http://www.jtcvsonline.org/article/S0022-5223(04)01162-6/pdf
-
307. Boodhwani M, Williams K, Babaev A, Gill G, Saleem N and Rubens FD. Ultrafiltration reduces blood transfusions following cardiac surgery: A meta-analysis, European Journal of Cardio-Thoracic Surgery 2006; 30(6):892-897. http://ejcts.oxfordjournals.org/content/30/6/892.full.pdf
-
308. Golab HD, Scohy TV, de Jong PL, Takkenberg JJ and Bogers AJ. Intraoperative cell salvage in infants undergoing elective cardiac surgery: a prospective trial, European Journal of Cardio-Thoracic Surgery 2008; 34(2):354-359. http://ejcts.oxfordjournals.org/content/34/2/354.full.pdf
-
309. Codispoti M and Mankad PS. Significant merits of a fibrin sealant in the presence of coagulopathy following paediatric cardiac surgery: randomised controlled trial, European Journal of Cardio-Thoracic Surgery 2002; 22(2):200-205. http://ejcts.oxfordjournals.org/content/22/2/200.full.pdf
-
310. Atkinson JB, Gomperts ED, Kang R, Lee M, Arensman RM, Bartlett RH, et al. Prospective, randomized evaluation of the efficacy of fibrin sealant as a topical hemostatic agent at the cannulation site in neonates undergoing extracorporeal membrane oxygenation, American Journal of Surgery 1997; 173(6):479-484. http://www.americanjournalofsurgery.com/article/S0002-9610(97)00018-4/abstract
-
311. CoStasis Multi-center Collaborative Writing C. A novel collagen-based composite offers effective hemostasis for multiple surgical indications: Results of a randomized controlled trial, Surgery 2001; 129(4):445-450. http://www.surgjournal.com/article/S0039-6060(01)81890-0/abstract
-
312. Sirlak M, Eryilmaz S, Yazicioglu L, Kiziltepe U, Eyileten Z, Durdu MS, et al. Comparative study of microfibrillar collagen hemostat (Colgel) and oxidized cellulose (Surgicel) in high transfusion-risk cardiac surgery, J Thorac Cardiovasc Surg 2003; 126(3):666-670. http://www.jtcvsonline.org/article/S0022-5223(03)00042-4/pdf
-
313. Chapman WC, Singla N, Genyk Y, McNeil JW, Renkens KL, Reynolds TC, et al. A phase 3, randomized, double-blind comparative study of the efficacy and safety of topical recombinant human thrombin and bovine thrombin in surgical hemostasis, Journal of the American College of Surgeons 2007; 205(2):256-265. http://www.journalacs.org/article/S1072-7515(07)00456-5/abstract
-
314. Weaver FA, Lew W, Granke K, Yonehiro L, Delange B, Alexander WA, et al. A comparison of recombinant thrombin to bovine thrombin as a hemostatic ancillary in patients undergoing peripheral arterial bypass and arteriovenous graft procedures, Journal of Vascular Surgery 2008; 47(6):1266-1273. http://www.jvascsurg.org/article/S0741-5214(08)00106-7/pdf
-
315. Lumsden AB, Heyman ER and Closure Medical Surgical Sealant Study G. Prospective randomized study evaluating an absorbable cyanoacrylate for use in vascular reconstructions, Journal of Vascular Surgery 2006; 44(5):1002-1009, discussion 1009. http://www.jvascsurg.org/article/S0741-5214(06)01213-4/pdf
-
316. Oz MC, Cosgrove DM, Badduke BR, Hill JD, Flannery MR, Palumbo R, et al. Controlled clinical trial of a novel hemostatic agent in cardiac surgery, The Annals of Thoracic Surgery 2000; 69(5): 1376-1382. http://www.annalsthoracicsurgery.org/article/S0003-4975(00)01194-2/pdf
-
317. Glickman M, Gheissari A, Money S, Martin J, Ballard JL and CoSeal Multicenter Vascular Surgery Study G. A polymeric sealant inhibits anastomotic suture hole bleeding more rapidly than gelfoam/thrombin: results of a randomized controlled trial, Archives of Surgery (Chicago, Ill.) 2002; 137(3):326-331, discussion 332. http://archsurg.jamanetwork.com/data/Journals/SURG/5348/soa1157.pdf
-
318. Saha SP, Muluk S, Schenk W, Dennis JW, Ploder B, Grigorian A, et al. A prospective randomized study comparing fibrin sealant to manual compression for the treatment of anastomotic suture-hole bleeding in expanded polytetrafluoroethylene grafts, Journal of Vascular Surgery 2012; 56(1):134-141. http://www.jvascsurg.org/article/S0741-5214(12)00077-8/pdf
-
319. Nasso G, Piancone F, Bonifazi R, Romano V, Visicchio G, De Filippo CM, et al. Prospective, randomized clinical trial of the FloSeal matrix sealant in cardiac surgery, The Annals of Thoracic Surgery 2009; 88(5):1520-1526. http://www.annalsthoracicsurgery.org/article/S0003-4975(09)01487-8/pdf
-
320. Fischer CP, Bochicchio G, Shen J, Patel B, Batiller J and Hart JC. A prospective, randomized, controlled trial of the efficacy and safety of fibrin pad as an adjunct to control soft tissue bleeding during abdominal, retroperitoneal, pelvic, and thoracic surgery, Journal of the American College of Surgeons 2013; 217(3):385-393. http://www.journalacs.org/article/S1072-7515(13)00325-6/abstract
-
321. Ferraris VA, Brown JR, Despotis GJ, Hammon JW, Reece TB, Saha SP, et al. update to the Society of Thoracic Surgeons and the Society of Cardiovascular Anesthesiologists blood conservation clinical practice guidelines, The Annals of Thoracic Surgery 2011; 91(3):944-982. http://www.annalsthoracicsurgery.org/article/S0003-4975(10)02888-2/pdf
-
322. Barnard J and Millner R. A review of topical hemostatic agents for use in cardiac surgery, The Annals of Thoracic Surgery 2009; 88(4):1377-1383. http://www.annalsthoracicsurgery.org/article/S0003-4975(09)00382-8/pdf
-
323. Achneck HE, Sileshi B, Jamiolkowski RM, Albala DM, Shapiro ML and Lawson JH. A comprehensive review of topical hemostatic agents: efficacy and recommendations for use, Annals of Surgery 2010; 251(2):217-228.
-
324. Gabay M and Boucher BA. An essential primer for understanding the role of topical hemostats, surgical sealants, and adhesives for maintaining hemostasis, Pharmacotherapy 2013; 33(9):935-955. http://onlinelibrary.wiley.com/doi/10.1002/phar.1291/abstract
-
325. Ozawa S. Patient blood management: use of topical hemostatic and sealant agents, AORN Journal 2013; 98(5):461-478. http://www.aornjournal.org/article/S0001-2092(13)00907-1/abstract
-
326. World Health Organization (WHO) (2008). Worldwide prevalence of anaemia 1993–2005: WHO global database on anaemia, WHO, Geneva.
-
327. Kassebaum NJ, Jasrasaria R, Naghavi M, Wulf SK, Johns N, Lozano R, et al. A systematic analysis of global anemia burden from 1990 to 2010, Blood 2014; 123(5):615-624. http://www.bloodjournal.org/content/123/5/615.long?sso-checked=true
-
328. Brewster DR. Iron deficiency in minority groups in Australia, J Paediatr Child Health 2004; 40(8):422-423. http://www.ncbi.nlm.nih.gov/pubmed/15265180
-
329. Bar-Zeev SJ, Kruske SG, Barclay LM, Bar-Zeev N and Kildea SV. Adherence to management guidelines for growth faltering and anaemia in remote dwelling Australian Aboriginal infants and barriers to health service delivery, BMC Health Services Research 2013; 13(250):1-12.
-
330. Aquino D, Marley JV, Senior K, Leonard D, Helmer J, Joshua A, et al. (2013). Early Childhood Nutrition and Anaemia Prevention Project: Executive summary, The Fred Hollows Foundation, Indigenous Australia Program, Darwin. http://www.kamsc.org.au/research/downloads/ECNAPP_Exec_Summary_for_web.pdf
-
331. Domellof M, Braegger C, Campoy C, Colomb V, Decsi T, Fewtrell M, et al. Iron requirements of infants and toddlers, J Pediatr Gastroenterol Nutr 2014; 58(1):119-129. http://www.ncbi.nlm.nih.gov/pubmed/24135983
-
332. Grant CC, Wall CR, Brewster D, Nicholson R, Whitehall J, Super L, et al. Policy statement on iron deficiency in pre-school-aged children, J Paediatr Child Health 2007; 43(7-8):513-521. http://www.ncbi.nlm.nih.gov/pubmed/17635678
-
333. European Society of Paediatric Gastroenterology Nutrition. Nutrition and feeding of preterm infants. Committee on Nutrition of the Preterm Infant, European Society of Paediatric Gastroenterology and Nutrition, Acta Paediatrica (Oslo, Norway). Supplement 1987; 336:1-14.
-
334. Cormack B (2003). Neonatal and Infant Nutrition Handbook, Auckland District Health Board, Auckland.
-
335. Australian National Health and Medical Research Council (NHMRC) and New Zealand Ministry of Health (MoH) (2006). Nutrient Reference Values for Australia and New Zealand Including Recommended Dietary Intakes, NHMRC and MoH.
-
336. Royal College of Pathologists of Australasia (RCPA) (2013). Iron studies standardised reporting protocol, RCPA, Sydney.
-
337. Ritchie B, McNeil Y and Brewster DR. Soluble transferrin receptor in Aboriginal children with a high prevalence of iron deficiency and infection, Tropical Medicine & International Health 2004; 9(1): 96-105.
-
338. Powers JM and Buchanan GR. Diagnosis and management of iron deficiency anemia, Hematol Oncol Clin North Am 2014; 28(4):729-745, vi-vii. http://www.ncbi.nlm.nih.gov/pubmed/25064710
-
339. Gastroenterological Society of Australia (2008.). Clinical update: Iron deficiency, First Edition, Digestive Health Foundation, Sydney. http://www.gesa.org.au
-
340. Pasricha SR, Flecknoe-Brown SC, Allen KJ, Gibson PR, McMahon PL, Olynyk JK, et al. Diagnosis and management of iron deficiency anaemia: a clinical update, Med J Aust 2010; 193(9): 525-532. http://www.ncbi.nlm.nih.gov/pubmed/21034387
-
341. Goddard AF, James MW, McIntyre AS, Scott BB and British Society of G. Guidelines for the management of iron deficiency anaemia, Gut 2011; 60(10):1309-1316. http://gut.bmj.com/content/60/10/1309.full.pdf
-
342. National Health and Medical Research Council (NHMRC) (2012). Infant feeding guidelines, NHMRC.
-
343. Point-of-care quick reference: Iron deficiency anemia, American Academy of Pediatrics. http://pediatriccare.solutions.aap.org/Quickreference.aspx?indexTypeId=9
-
344. Paediatric Pharmacopoiea (2002). Pocket prescriber (13th Edition), 13th ed, Pharmacy Department, The Royal Children’s Hospital (RCH), Melbourne, Australia.
-
345. Crary SE, Hall K and Buchanan GR. Intravenous iron sucrose for children with iron deficiency failing to respond to oral iron therapy, Pediatr Blood Cancer 2011; 56(4):615-619. http://onlinelibrary.wiley.com/doi/10.1002/pbc.22930/abstract
-
346. Laass MW, Straub S, Chainey S, Virgin G and Cushway T. Effectiveness and safety of ferric carboxymaltose treatment in children and adolescents with inflammatory bowel disease and other gastrointestinal diseases, BMC Gastroenterol 2014; 14:184. http://www.ncbi.nlm.nih.gov/pubmed/25326048}
-
347. Pinsk V, Levy J, Moser A, Yerushalmi B and Kapelushnik J. Efficacy and safety of intravenous iron sucrose therapy in a group of children with iron deficiency anemia, The Israel Medical Association Journal 2008; 10(5):335-338.
-
348. Tenenbein M and Rodgers GC. The four A’s of decreasing the toll of childhood iron poisoning deaths, Archives of Family Medicine 1994; 3(9):754-755.
-
349. Hendrickson JE, Shaz BH, Pereira G, Atkins E, Johnson KK, Bao G, et al. Coagulopathy is prevalent and associated with adverse outcomes in transfused pediatric trauma patients, J Pediatr 2012; 160(2):204-209 e203. http://www.ncbi.nlm.nih.gov/pubmed/21925679
-
350. Hendrickson JE, Shaz BH, Pereira G, Parker PM, Jessup P, Atwell F, et al. Implementation of a pediatric trauma massive transfusion protocol: one institution’s experience, Transfusion 2012; 52(6):1228-1236. http://www.ncbi.nlm.nih.gov/pubmed/22128884
-
351. Chidester SJ, Williams N, Wang W and Groner JI. A pediatric massive transfusion protocol, J Trauma Acute Care Surg 2012; 73(5):1273-1277. http://www.ncbi.nlm.nih.gov/pubmed/23064608
-
352. Dressler AM, Finck CM, Carroll CL, Bonanni CC and Spinella PC. Use of a massive transfusion protocol with hemostatic resuscitation for severe intraoperative bleeding in a child, J Pediatr Surg 2010; 45(7):1530-1533. http://www.ncbi.nlm.nih.gov/pubmed/20638538
-
353. Diab YA, Wong EC and Luban NL. Massive transfusion in children and neonates, Br J Haematol 2013; 161(1):15-26. http://www.ncbi.nlm.nih.gov/pubmed/23432321